| History of Plague |
| Plague’s deadly epidemic potential is notorious and well documented. The Justinian pandemic (542 to 767 A.D.) spread from central Africa to the Mediterranean littoral and thence to Asia Minor, causing an estimated 40 million deaths. The second pandemic began in central Asia, was carried to Sicily by ship from Constantinople in 1347, and swept through Europe and the British Isles in successive waves over the next four centuries. At its height, it killed as many as a quarter of the affected population and became known as the Black Death.In the third (modern) pandemic, plague appeared in Yunnan, China, in the latter half of the nineteenth century; established itself in Hong Kong in 1894; and spread by ship to Bombay in 1896 and subsequently to major port cities throughout the world, including San Francisco and several other West Coast and Gulf Coast ports in the United States. The plague bacillus was first cultured by Alexandre Yersin in Hong Kong in 1894. In 1898, Paul-Louis Simond, a French scientist sent to investigate epidemic bubonic plague in Bombay, identified the bacillus in the tissues of dead rats and proposed transmission by rat fleas. Waldemar Haffkine, also in Bombay at that time, developed a crude vaccine.
By 1910, plague had circled the globe and established itself in rodent populations on all inhabited continents other than Australia. After 1920, however, the spread of plague was largely halted by international regulations that mandated control of rats in harbours and inspection and rat-proofing of ships. Before the third pandemic subsided, it resulted in an estimated 26 million plague cases and more than 12 million deaths, the vast majority in India. By 1950, plague outbreaks around the world had become isolated, sporadic, and manageable with modern techniques of surveillance, flea and rat control, and antimicrobial treatment of patients. From 1969 through 1993, a median of 1356 human plague cases were reported annually to the World Health Organization, with around 10 to 15 countries reporting cases each year. Plague has practically disappeared from cities and now occurs mostly in rural and semirural areas, where it is maintained in wild rodents. In the United States, the last outbreak of urban plague occurred in Los Angeles in 1924 and 1925, and human cases since then have resulted from zoonotic exposures in rural areas of western states. Plague, because of its pandemic history, remains one of three quarantinable diseases subject to international health regulations (the other two being cholera and yellow fever). The alarm that plague is still able to evoke was highlighted by the public panic over and exaggerated international response to reports of outbreaks of bubonic and pneumonic plague in India in 1994. Except for large outbreaks of pneumonic plague in Manchuria in the early part of the twentieth century, person-to-person respiratory transmission of plague during and since the third pandemic has occurred only sporadically and has been limited to clusters of close contacts of pneumonic plague patients, such as household members and caregivers. The 1994 outbreak of pneumonic plague in the city of Surat, India, although reported to be extensive, most likely involved fewer than 100 cases and 50 deaths. From 1979 through 1993, 16,312 human plague cases and 1668 deaths (mortality, 10 percent) were reported by 20 countries to the World Health Organization. In the same 15-year period, the United States reported 227 plague cases (mean, 15 cases per year) and 32 deaths (mortality, 14 percent). |
| Plague |
Tag Archives: Plague
Plague
| Plague | ||
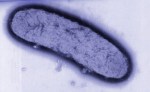
| Plague is one of the most virulent and potentially lethal diseases known. It is caused by an organism called Yersinia pestis.Y. pestis is a gram-negative coccobacillus in the family Enterobacteriaceae. It is a zoonotic disease and its usual hosts are rodents.It is transmitted to humans usually by flea bite and less commonly by direct contact with infected animal tissues or by airborne droplet. | ||
 |
 |
 |
| The clinical forms of plague are bubonic, septicemic, and pneumonic. Most cases are sporadic, occurring singly or in small clusters, although the potential for epidemic spread still exists in some countries.Y. pestis organism is maintained in animal cycles involving relatively resistant wild rodents and their fleas. Humans and other non-rodent mammals are incidental hosts, that is they just happen to get involved.
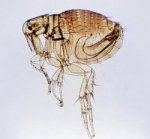
Transmission involving susceptible rodents and flea results in local or even widespread death of susceptible rodents and poses a more serious threat to humans. In the United States, the principal animal hosts are various ground squirrels, prairie dogs, and chipmunks. Y. pestis occasionally spills over from wild rodents to commensal rat species that inhabit cultivated fields and adjacent homes, villages, and towns. The organism can then be transported from towns to cities by these relatively cosmopolitan rats and their fleas. Plague in populated areas is most likely to develop when sanitation is poor and rats are numerous, especially the common black or roof rat (Rattus rattus) and the larger brown sewer or Norway rat (R. norvegicus). A high mortality rate from plague in these susceptible rat populations forces their fleas to seek alternative hosts, including humans. The oriental rat flea Xenopsylla cheopis and (in southern Africa and Brazil) the related species X. brasiliensis are efficient vectors of the plague bacillus among rats and are also efficient vectors to humans. |
| Except for large outbreaks of pneumonic plague in Manchuria in the early part of the twentieth century, person-to-person respiratory transmission of plague has occurred only sporadically and has been limited to clusters of close contacts of pneumonic plague patients, such as household members and caregivers. The 1994 outbreak of pneumonic plague in the city of Surat, India, although reported to be extensive, most likely involved fewer than 100 cases and 50 deaths. |
| Plague can be transmitted during the skinning and handling of carcasses of wild animals such as rabbits and hares, prairie dogs, wildcats.Carnivores, including dogs and cats, can become infected with Y. pestis by eating infected rodents and perhaps by being bitten by fleas from infected rodents. Although clinical plague commonly develops in infected cats, it rarely does so in infected dogs, which thus do not directly expose humans to infection. However, both dogs and cats may transport infected fleas from rodent-infested areas to the home environment. |
|
Clinical Features |
| Plague is characterized by a rapid onset of fever and other systemic manifestations. If it is not quickly and correctly treated, plague can follow a toxic course, resulting in shock, multiple-organ failure, and death.In humans, the three principal forms of plague are bubonic, septicemic, and pneumonic. Bubonic plague, the most common form, is almost always caused by the bite of an infected flea but occasionally results from direct inoculation of infectious tissues or fluids. Septicemic and pneumonic plague can be either primary or secondary to metastatic spread.
Bubonic plague usually has an incubation period of 2 to 6 days, occasionally longer. The patient experiences chills, fever; myalgias; arthralgias; headache; and a feeling of weakness. Soon usually within 24 h the patient notices tenderness and pain in one or more regional lymph nodes proximal to the site of inoculation of the plague bacillus. Because fleas often bite the legs, femoral and inguinal nodes are most commonly involved; axillary and cervical nodes are next most commonly affected. The enlarging bubo becomes progressively painful and very tender. The surrounding tissue often becomes oedematous, sometimes markedly so, and the overlying skin may be erythematous, warm, and tense. Inspection of the skin surrounding or distal to the bubo sometimes reveals the site of a flea bite marked by a small papule, pustule, scab, or ulcer. Septicaemic plague is a progressive, overwhelming bacterial infection. Primary septicemia develops in the absence of regional lymphadenitis. Patients with septicemic plague often present with gastrointestinal symptoms of nausea, vomiting, diarrhea, and abdominal pain. If not treated early with appropriate antibiotics, septicemic plague can be fulminant and fatal. Pneumonic plague develops most rapidly and is most frequently fatal. Pneumonic plague arises from exposure to infective respiratory droplets from a person or cat with respiratory plague or secondary to hematogenous spread in a patient with bubonic or septicemic plague. Pneumonic plague can also result from accidental inhalation of Y. pestis in the laboratory. The incubation period for primary pneumonic plague is rarely longer than 1 to 4 days. The onset is most often sudden, with chills, fever, headache, myalgias, weakness, and dizziness. Pulmonary signs, including cough, sputum production, chest pain, tachypnea, and dyspnea, typically arise on the second day of illness and may be accompanied by haemoptysis, increasing respiratory distress, and circulatory collapse. Prevention A killed, whole-cell plague vaccine is available in the United States. Primary immunization consists of a series of three injections followed by booster doses as warranted (at intervals of 6 months or more) Treatment Streptomycin is the drug of choice. Alternative antibiotics include the Tetracyclines and Chloramphenicol. |
| History of Plague |
