| Psoriasis ~ Treatment | |
| Although there is no known cure of psoriasis, the disease can be effectively controlled by various treatment modalities.The mainstay of topical treatment of psoriasis is coal tar which was made popular by Goeckerman in 1925. Used for 8-10 hrs. (1%,5%,25%) is very effective.Majority of the patients respond to topical therapy which includes emollients, keratolytics, coal tar, anthralin and corticosteroids. The newer agents are topical PUVA, Topical Methotrexate, Calcipotriol and Tazarotene (a retinoid).Coal Tar preparations: 100 % strong coal tar solution and 4 % tar paste are to be applied to the patches twice daily. Salicylic acid 1-2 % may be added to the preparation to remove scaling. Dithranol: 1-2 % dithranol cream is applied to the lesions for duration of 30 minutes daily. Coal tar and Dithranol preparation are best avoided on face, genitals and skin folds as they are irritating. Topical Steroids: Their long term use is not indicated in most cases as on their withdrawal relapse may occur and the disease may change to unstable phase. Indications of their use are lesions of face, genitals and skin flexures where coal tar may be too irritant. Unresponsive lesions of scalp and soles may also need topical steroids. Ultraviolet radiation: Natural sunlight has beneficial effect. During winters medium wave ultraviolet radiation is helpful. Systemic treatment: In extensive psoriasis which fails to respond with local measures may need to be put on systemic treatment considering the side effects as they have to be taken for long period. Psoralen, Retinoids (etretinate), Methotrexate have to be given along with local medication. |
|
| METHOTREXATE is a Most-effective treatment of psoriasis that is widespread, covering large areas of the body, and resistant to conventional topical therapy, according to Dr. Inderjeet Kaur, Associate Professor, Department of Dermatology, Venereology and Leprology, Postgraduate Institute of Medical Education and Research, Chandigarh.In 82 selected patients with psoriasis at the PGI, methotrexate (MTX) led to clearance of the lesions in nearly 80% in a mean period of 8 weeks, Dr. Kaur said in the Fulford oration at the 26th annual conference of the Indian Association of Dermatology, Venereology and Leprology.With the stringent precautions taken, MTX therapy did not provoke adverse side effects such as hepatotoxicity, even when used in children and elderly patients to control severe disease episodes. | |
| Palmo Plantar PsoriasisTreatment of PPP which causes severe handicaps both cosmetically and functionally presents particular challenge.MTX gel 1 % was used twice daily for 8 wks. Good improvement was found in 80% of palmar and 64% of planter lesions. Topical MTX if used in a suitable vehicle that enhances percutaneous absorption and if used for a sufficient length of time has beneficial effect on PPP. | 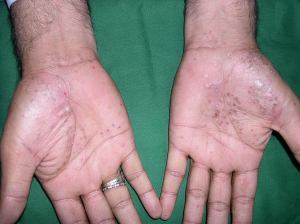 |
| Topical PUVASOL : The palms and soles of the patient was submerged in an 8-MOP soak solution for 15 minutes, followed by sun exposure immediately after drying. The treatment was given twice weekly for 8 weeks. 70 % palmar and 27 % planter cases show good improvement. Only one patient had phototoxic reaction. PUVASOL is effective and safe therapy for palmar psoriasis.Coal – tar therapy: 6 % crude coal tar (CCT), when used under occlusion, resulted in good improvement in 77 % of PPP patients.Calcipotriol: Calcipotriol ointment 50 micg/g was used every night under occlusion for 8 weeks. Excellent improvement was seen in the palms. | 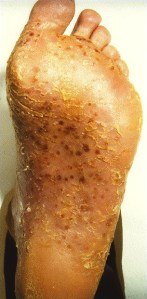 |
|
Systemic Treatment Systemic treatment is reserved for patients with extensive disease or on whom conventional therapy has failed. Systemic therapy include PUVA, Conticosteroids, MTX, Hydroxyurea, Cyclosporine and Calcipotriol. Before starting systemic therapy, patients undergo complete clinical and laboratory evaluation and only those with near normal renal, hepatic and marrow function are selected to receive MTX. In the PGI series, 82 patients were given a single oral weekly dose of 0.4-0.6 mg/kg body weight of MTX. Nearly 80% clearance was seen in a mean period of 8 weeks. The drug could he completely withdrawn in 90% patients, coinciding with the seasonal remission. There was no response in 2 patients. The commonest side effects were nausea and vomiting, which occurred in 30% patients. Post- MTX disease free interval was 7.7 months. The drug had to be restarted in 13 patients while the others could be managed with topical therapy in the subsequent relapses. MTX-free period of 4-6 months reduces the drug’s hepatoxicity. MTX has also been used safely and effectively in children and elderly patients to control severe episodes of the disease. |
|
|
Other systemic drugs tried included Mesalazine, effective in about one-third of the patients, oral Nystatin, found to be ineffective, and cyclosporine, used in selected cases to tide over a crisis. Corticosteroids were found to have no role in routine treatment of psoriasis because of the risk of rebound. |
|
| FDA OKs mousse to treat psoriasis Patients who suffer psoriasis of the scalp won a slightly different kind of treatment a mousse-like foam to rub onto scalp lesions with less mess than traditional drugs. Until now, the main treatment has been a lotion containing the chemical betamethasone, but putting a lotion on the scalp every day is messy and greasy. The Food and Drug Administration approved Connetics Corp.’s new version of betamethasone, an easier-to-apply foam called Luxiq. An estimated 3.5 million Americans have scalp psoriasis, marked by redness, scaling, severe itching and irritation. In one study of 172 patients, 72% treated with Luxiq had complete or almost complete clearance of their psoriasis outbreak, compared with 47% who used a betamethasone lotion. |
|
