| Conditions associated with Osteoporosis |
|

| Conditions associated with Osteoporosis |
|
| Role of Oestrogen in Osteoporosis |
| The Role of Hormone Therapy in the Prevention and Treatment of OsteoporosisWhile one in four women over the age of 50 has osteoporosis, only one in eight men have the disease. This striking difference is largely due to the important role which the sex hormones (primarily estrogen) play in keeping women’s bones healthy. |
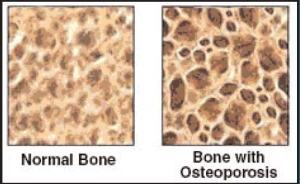
| Bone is a living tissue that is constantly renewed through a process in which old bone is removed and replaced by new bone. In Bone there are two important types of cells – Osteoblasts and Osteoclasts. Osteoclasts are bone eroding cells and Osteoblasts are bone forming cells. The bone eroding cells invade the bone and erode it creating cavities in the bone and the bone forming cells fill the cavities with new bone. This is a natural process — nature’s way of restoring bones and keeping them strong. In younger persons with good bone health, both the cells that erode bone and those that build bone work together. But as we age the bone builders are unable to keep pace with the bone excavators, and this results in loss of bone. |
|
| Calcium & Vitamin D ~ An Essential Element for Bone Health |
| Importance of Calcium There is strong and convincing evidence that calcium is important for building strong bones in childhood, maintaining bone density in adults, and reducing the likelihood of fractures as we age.
Calcium is crucial for life. Every cell in the body needs calcium to function properly. Heart, Nerve and Muscles all need calcium for their activity. Bones need calcium to maintain strength. 99 % of body calcium is in the bones. Our Body gets calcium from food we eat. If dietary source is deficient in calcium, our body gets it from our bones. Calcium is essential for bony health for number of reasons. In childhood it is needed for proper formation of bony skeleton to support growing body. By the age 20 bones stop growing in length and by this time peak bony mass is reached. The density of your bones at this point will depend, in part, upon the extent of your calcium intake as a child. The greater this peak bone mass, the less likely your bones are to become porous and fragile later on. |
| Bone is living tissue, constantly renewing itself. Daily wear and tear causes structural defects which need to be taken care of. This process in the bones is termed as Bone remodelling. Remodelling is an ongoing, natural process and the cycle is completed every three to four months in a healthy young adult. With age this maintenance system becomes less efficient. In people who have relatively healthy bones, adequate calcium intake can help the remodelling process stay balanced. This means that replacement of new bone will remain more efficient, thus preventing a rapid decline in density. |
| Calcium and Menopause Calcium is especially important at menopause because calcium absorption seems to slow down with the decrease in estrogen. |
| How Much Calcium Do You Need? Following nutritional intake of calcium every day is essential, to maintain strong bones. |
|
Recommended Daily Calcium Intake |
| Infants birth-6 months – 400 mg / day 6-12 months – 600 mg / day |
| Children 1-5 years – 800 mg / day 6-11 years – 800-1200 mg / day |
| Adolescents & Young adults 11-24 years – 1200-1500 mg / day |
| Women 25-50 years – 1000 mg / day Pregnant or lactating women – 1200-1500 mg / day Postmenopausal women on estrogen – 1000 mg / day Postmenopaural women not on estrogen – 1500 mg / day |
| Men (25-50 years) – 1000 mg / day |
| All women and men above 65 – 1500 mg / day |
| Is There Such a Thing as Too Much Calcium?No adverse effects have been observed in people who consume well above the recommended daily intake of calcium (up to 2500 mg per day). A high dietary intake of calcium used to be suspected of increasing the risk of kidney stones, but most experts now believe that this is incorrect. |
| Osteoporosis ~ Diagnosis | |||||||||||||||||||||||||||||||
| To diagnose Osteoporosis we have to find out the calcium content of the bones. To put it more scientifically, the Bone Mineral Density ( BMD) has to be evaluated. The technology that is used to do this is known as Bone Densitometry. Before the advent of BMD tests, osteoporosis was diagnosed by routine X-rays or by bone biopsy. By these methods osteoporosis could be rarely diagnosed before at least 25 % of the bone mass was lost, and by this time the disease is well advanced. Today BMD tests help in diagnosing the disease and also help in warning us from the likely hood of developing osteoporosis in the near future. |
|||||||||||||||||||||||||||||||
| Indications for BMD tests 1. At Menopause, to decide regarding the need for Hormone therapy. 2. Those on glucocorticoids, to see if they are losing bone mass or not. 3. Recent fractures, where osteoporosis is suspected. 4. Those with osteoporosis and under treatment, to monitor the effectiveness of treatment. 5. Those with Primary Hyperparathyroidism. 6. A man with Hypogonadism. 7. Those on chemotherapy and may be losing bone mass. |
 |
||||||||||||||||||||||||||||||
| The most common bone density test in use today is called dual energy x-ray absorptiometry (DXA). It is a non invasive procedure and the amount of radiation exposure is very little.The results are expressed in units referred to as standard deviations (SD). These SD units tell how far you differ (or deviate) from what is considered normal. If you are 2.5 SD units below normal (-2.5), you will be told that you have osteoporosis. |
|||||||||||||||||||||||||||||||
| Heel Ultrasound: A new Technology for testing Bone Density The test usually involves immersing your foot in a bath of warm water, allowing high frequency sound waves to pass through your heel. The test measures the density and quality of the bone in your heel. It has not yet become a standard testing procedure.
|
|||||||||||||||||||||||||||||||
|
Recommended Daily Calcium Intake |
| Infants birth-6 months – 400 mg / day 6-12 months – 600 mg / day |
| Children 1-5 years – 800 mg / day 6-11 years – 800-1200 mg / day |
| Adolescents & Young adults 11-24 years – 1200-1500 mg / day |
| Women 25-50 years – 1000 mg / day Pregnant or lactating women – 1200-1500 mg / day Postmenopausal women on estrogen – 1000 mg / day Postmenopaural women not on estrogen – 1500 mg / day |
| Men (25-50 years) – 1000 mg / day |
| All women and men above 65 – 1500 mg / day |