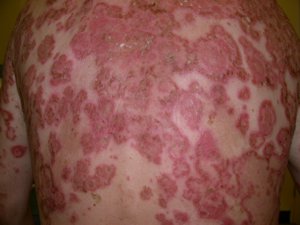
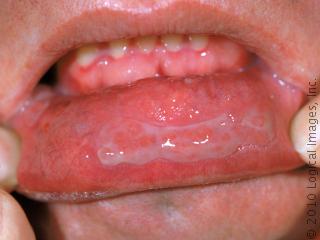
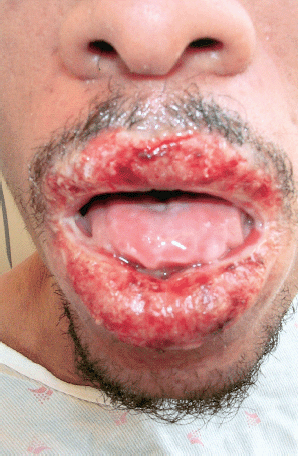
| Plague’s deadly epidemic potential is notorious and well documented. The Justinian pandemic (542 to 767 A.D.) spread from central Africa to the Mediterranean littoral and thence to Asia Minor, causing an estimated 40 million deaths. The second pandemic began in central Asia, was carried to Sicily by ship from Constantinople in 1347, and swept through Europe and the British Isles in successive waves over the next four centuries. At its height, it killed as many as a quarter of the affected population and became known as the Black Death.In the third (modern) pandemic, plague appeared in Yunnan, China, in the latter half of the nineteenth century; established itself in Hong Kong in 1894; and spread by ship to Bombay in 1896 and subsequently to major port cities throughout the world, including San Francisco and several other West Coast and Gulf Coast ports in the United States. The plague bacillus was first cultured by Alexandre Yersin in Hong Kong in 1894. In 1898, Paul-Louis Simond, a French scientist sent to investigate epidemic bubonic plague in Bombay, identified the bacillus in the tissues of dead rats and proposed transmission by rat fleas. Waldemar Haffkine, also in Bombay at that time, developed a crude vaccine.
By 1910, plague had circled the globe and established itself in rodent populations on all inhabited continents other than Australia. After 1920, however, the spread of plague was largely halted by international regulations that mandated control of rats in harbours and inspection and rat-proofing of ships. Before the third pandemic subsided, it resulted in an estimated 26 million plague cases and more than 12 million deaths, the vast majority in India. By 1950, plague outbreaks around the world had become isolated, sporadic, and manageable with modern techniques of surveillance, flea and rat control, and antimicrobial treatment of patients. From 1969 through 1993, a median of 1356 human plague cases were reported annually to the World Health Organization, with around 10 to 15 countries reporting cases each year. Plague has practically disappeared from cities and now occurs mostly in rural and semirural areas, where it is maintained in wild rodents. In the United States, the last outbreak of urban plague occurred in Los Angeles in 1924 and 1925, and human cases since then have resulted from zoonotic exposures in rural areas of western states.
Plague, because of its pandemic history, remains one of three quarantinable diseases subject to international health regulations (the other two being cholera and yellow fever). The alarm that plague is still able to evoke was highlighted by the public panic over and exaggerated international response to reports of outbreaks of bubonic and pneumonic plague in India in 1994.
Except for large outbreaks of pneumonic plague in Manchuria in the early part of the twentieth century, person-to-person respiratory transmission of plague during and since the third pandemic has occurred only sporadically and has been limited to clusters of close contacts of pneumonic plague patients, such as household members and caregivers. The 1994 outbreak of pneumonic plague in the city of Surat, India, although reported to be extensive, most likely involved fewer than 100 cases and 50 deaths.
From 1979 through 1993, 16,312 human plague cases and 1668 deaths (mortality, 10 percent) were reported by 20 countries to the World Health Organization. In the same 15-year period, the United States reported 227 plague cases (mean, 15 cases per year) and 32 deaths (mortality, 14 percent). |


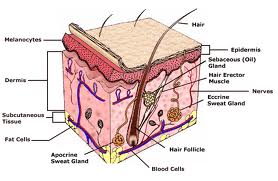 However, it is mainly determined by melanin, a pigment manufactured by dendritic cells called melanocytes, found among the basal cells of the epidermis. Their numbers in any one region of the body, range from about 1,000- 2,000 per square millimetre. It is roughly the same within and between races. The blondest whites have as many as the darkest blacks. Colour differences are due solely to the amount of melanin produced and the nature of the pigment granules. When the skin becomes tanned on exposure to sunlight, the melanocytes do not increase in number, only in activity. Not only do melanocytes produce a tan, they are also responsible for the form of cancer called melanoma. Melanoma is caused by UV radiation damage to melanocytes.
However, it is mainly determined by melanin, a pigment manufactured by dendritic cells called melanocytes, found among the basal cells of the epidermis. Their numbers in any one region of the body, range from about 1,000- 2,000 per square millimetre. It is roughly the same within and between races. The blondest whites have as many as the darkest blacks. Colour differences are due solely to the amount of melanin produced and the nature of the pigment granules. When the skin becomes tanned on exposure to sunlight, the melanocytes do not increase in number, only in activity. Not only do melanocytes produce a tan, they are also responsible for the form of cancer called melanoma. Melanoma is caused by UV radiation damage to melanocytes.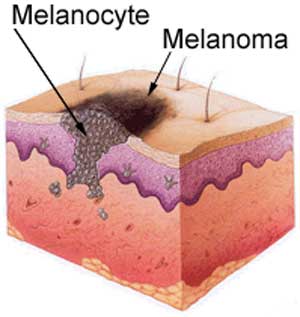 squamous cell carcinoma and
squamous cell carcinoma and  Castor beans are processed throughout the world to make castor oil. Ricin is part of the waste “mash” produced when castor oil is made.It can be in the form of a powder, a mist, or a pellet, or it can be dissolved in water. It is a stable substance under normal conditions, but can be inactivated by heat above 80 degrees Centigrade.
Castor beans are processed throughout the world to make castor oil. Ricin is part of the waste “mash” produced when castor oil is made.It can be in the form of a powder, a mist, or a pellet, or it can be dissolved in water. It is a stable substance under normal conditions, but can be inactivated by heat above 80 degrees Centigrade.