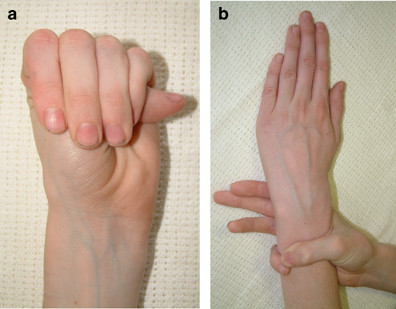
Osteogenesis Imperfecta
Synonyms:
- Brittle Bone Disease
- Ekman-Lobstein Disease
- Lobstein Disease (Type I)
- OI
- Vrolik Disease (Type II)
OI occurs about once in every 10,000 births and the incidence is about the same worldwide.
Osteogenesis Imperfecta is a group of disease characterized by extremely fragile bones that break easily often without any apparent cause. This disease is due to the abnormality of the connective tissue and it is a genetic disorder. In most cases, the various forms of osteogenesis imperfecta are inherited as Autosomal dominant traits.
The mutation is found on the COL1A2 gene on the long arm of chromosome 7 and/or the COL1A1 gene on the long arm of chromosome 17.
Four main types of OI have been identified. OI type I is the most common and the mildest form of the disorder. OI type II is the most severe. The symptoms of OI vary greatly from case to case and even among members of the same family. A person may have just a few or several hundred fractures in a lifetime.
Some of the features seen in patients of OI are
- Stature is may be normal in mild forms. But in severe form (Type II ) body stature is small with underdeveloped lungs.
- Type II variety is lethal shortly after birth.
- Loose joints and low muscle tone.
- Tendency towards spinal curvature.
- Brittle teeth.
- Sclera (white of eye) has blue, purple or gray tint.
- Hearing loss may be present starting in 20s or 30s.
- Collagen may be normal in Type I with amount less than normal. In other types the collagen in improperly formed.
- Triangular face.


Most cases of OI are caused by autosomal dominant genetic defect. Some children with OI inherit the disorder from a parent. Other children are born with OI even though there is no family history of the disorder. In these children, the genetic defect occurred as a spontaneous mutation. A person with OI has 50% chance of passing the disorder to his or her children.
there is no family history of the disorder. In these children, the genetic defect occurred as a spontaneous mutation. A person with OI has 50% chance of passing the disorder to his or her children.
The prognosis for this disease depends on various factors especially the severity of the symptoms. Despite disability most of the persons lead productive life.
There is no cure yet for this disease. The main management involves around managing symptoms, preventing fractures, developing optimal bone and muscle mass, maximizing mobility.
Rodding surgery is frequently used in OI patients. In this procedure metal rod is inserted through the length of long bones to prevent and correct deformities and strengthen the bones.
Persons with OI should exercise as much as possible. The best exercise is swimming and walking. It is advisable to maintain healthy weight have nutritious diet and avoid intoxicants.

 (mutations) that occur randomly for no apparent reason. A rare form of Russell-Silver Syndrome is thought to be inherited as an X-linked dominant genetic trait.
(mutations) that occur randomly for no apparent reason. A rare form of Russell-Silver Syndrome is thought to be inherited as an X-linked dominant genetic trait.