|
Recommended Daily Calcium Intake |
| Infants birth-6 months – 400 mg / day 6-12 months – 600 mg / day |
| Children 1-5 years – 800 mg / day 6-11 years – 800-1200 mg / day |
| Adolescents & Young adults 11-24 years – 1200-1500 mg / day |
| Women 25-50 years – 1000 mg / day Pregnant or lactating women – 1200-1500 mg / day Postmenopausal women on estrogen – 1000 mg / day Postmenopaural women not on estrogen – 1500 mg / day |
| Men (25-50 years) – 1000 mg / day |
| All women and men above 65 – 1500 mg / day |
Author Archives: Manbir & Gurpreet
Calcium in Food
| Calcium in Food | |
| When considering food items rich in Calcium content it is important to select foods that contain easily absorbable calcium. The more easily calcium is absorbed; the more available it is to be used by the body. It is well accepted that dairy products such as milk, cheese and yogurt are the best sources of calcium because they contain high amounts of calcium, and the calcium is well absorbed by the body. |  |
| Skim milk products provide as much calcium as whole milk with the added advantages of less fat and cholesterol. |  |
| Dairy products such as milk,cheese and yogurt are the best sources of calcium because they contain high amounts of calcium, and the calcium is well absorbed by the body. |  |
| Bones in fish especially those of salmon and sardines, too contain useful calcium. |  |
| Vegetables such as broccoli, collards, kale, mustard greens, turnip greens, and bok choy, also contain calcium that is easily absorbed. These vegetables, however, contain smaller quantities of calcium per serving than dairy foods. |  |
| It is possible for foods to contain calcium and for that calcium to have limited availability to the body. The reason is that these foods contain calcium-binding substances called oxalates (found in many green vegetables) or phytates (found in unleavened grain products). Of these two substances, oxalates are considered more potent in their ability to restrict calcium absorption |  |
| While spinach contains calcium, it also contains oxalates, as do beet greens, chard, and rhubarb, that bind with calcium and interfere with its absorption. Even though the substances contained in these foods inhibit calcium absorption, experts agree that the benefits you derive from the other important nutrients contained in this group of foods far outweigh the negative effects of their tendency to block calcium absorption.Calcium loss through the urine is increased by excess consumption of salt, caffeine and protein. |  |
| Vitamin D for Calcium Absorption
Vitamin D is crucial to calcium absorption. In fact, it increases calcium |
|
Calcium Content of Some Common Food Items
| Calcium Content of Some Common Foods | Portion | Calcium |
| Milk and milk products | ||
| Cheese – Swiss, Gruyère | 1.75 oz./50 g | 493 mg |
| Cheese – Brick, Cheddar, Colby, Edam, Gouda | 1.75 oz./50 g | 353 mg |
| Milk – whole, 2%, 1%, skim | 1 glass/250 ml | 315 mg |
| Buttermilk | 1 glass/250 ml | 301 mg |
| Cheese – Mozzarella | 1.75 oz./50 g | 269 mg |
| Yogurt – plain | 1 cup/175 ml | 292 mg |
| Milk – powder, dry | 3 tbs./45 ml | 159 mg |
| Ice cream | 1/2 cup/125 ml | 93 mg |
| Cheese – cottage, creamed, 2%, 1% | 1/2 cup/125 ml | 87 mg |
| Meat, fish, poultry and alternatives | ||
| Sardines, with bones | 8 small | 153 mg |
| Salmon, with bones – canned | 1/2 – 213g can | 242 mg |
| Almonds | 1/2 cup/125ml | 200 mg |
| Sesame seeds | 1/2 cup/125ml | 100 mg |
| Beans – cooked (kidney, navy, pinto, garbanzo) | 1 cup/250 ml | 90 mg |
| Soybeans – cooked | 1 cup/250 ml | 175 mg |
| Chicken – roasted | 3 oz./90 g | 13mg |
| Beef – roasted | 3 oz./90 g | 7 mg |
| Tofu – with calcium sulfate | 1/2 cup/125ml | 130 mg |
| Breads and cereals | ||
| Muffin – bran | 1/35 g | 50 mg |
| Bread – white and whole wheat | 1 slice/30 g | 25 mg |
| Fruits and vegetables | ||
| Broccoli – raw | 1/2 cup/125ml | 38 mg |
| Orange | 1medium/180g | 52 mg |
| Banana | 1medium/175g | 10 mg |
| Lettuce | 2 large leaves | 8 mg |
| Figs – dried | 10 | 270 mg |
| Combination dishes | ||
| Lasagna – homemade | 1 cup/250 ml | 286 mg |
| Soup made with milk, such as cream of chicken, mushroom, tomato or broccoli | 1 cup/250 ml | 189 mg |
| Baked beans — canned | 1 cup/250 ml | 163 mg |
Osteoporosis – Risk Factors
| Osteoporosis – Risk Factors |
The following conditions predispose to loss of bone and increased susceptibility to osteoporosis and consequent fractures.
|
| Conditions associated with Osteoporosis |
Osteoporosis
| Osteoporosis | |
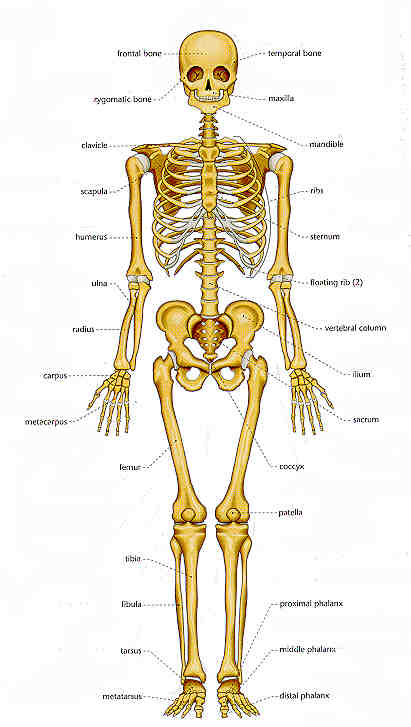
| Bone is living tissue, not a lifeless structure, that only supports your muscles and flesh. In fact, bone, like other body tissue, changes throughout a person’s life.Bone tissue is constantly renewed through a process called remodelling in which old bone is removed and replaced by new bone. This remodelling is a natural, ongoing process that takes place in a healthy body. It is Nature’s way of seeing that old bone is discarded and replaced with new bone. Loss in bone occurs because, as we age, new bone is not laid down at the same rate as older bone is lost; the result may be a thinning of the bones, referred to as Osteoporosis.Osteoporosis is characterized by low bone mass and deterioration of bone tissue.WHO defines osteoporosis as a marked reduction in bone density, to differentiate it from osteopenia which refers to mild reduction in bone density. In osteoporosis, the bone density is more than 2.5 standard deviations below the young normal mean (T scale <-2.5).Osteoporosis is often known as the silent thief because bone loss occurs without symptoms.True osteoporosis causes bone pain and or spontaneous fractures of the spine, hip and wrist. Osteoporosis is usually asymptomatic until fracture develops. Older persons with a fracture, especially spontaneous fracture of the spine, wrist or femur should be investigated for osteoporosis. |
 |
| Prevalence One in four women over the age of 50 has osteoporosis. One in eight men over 50 also has the disease. However, the disease can strike at any age. More women die each year as a result of osteoporotic fractures than from breast and ovarian cancer combined. A fifty-year-old woman has at least a 40 per cent risk of an osteoporotic fracture during the remainder of her life. Up to 20 per cent of individuals, who fracture a hip, die as a result of complications. Fifty per cent of those who survive remain permanently disabled. |
|
Osteoporosis related topics |
|

 absorption by as much as 30% to 80%. Adults should get 400 IUs of vitamin D per day (older adults should receive between 400 and 800).The easiest and most natural way to get Vitamin D is from exposure to sunlight, which causes the body to manufacture its own. Just 15 minutes a day of summer sun exposure, even if only on the arms, face and hands will greatly enhance Vitamin D production.
absorption by as much as 30% to 80%. Adults should get 400 IUs of vitamin D per day (older adults should receive between 400 and 800).The easiest and most natural way to get Vitamin D is from exposure to sunlight, which causes the body to manufacture its own. Just 15 minutes a day of summer sun exposure, even if only on the arms, face and hands will greatly enhance Vitamin D production. Although there are few food sources of Vitamin D, milk does contain significant amounts. (Fortified with Vitamin D, it contains 100 IUs per 250 ml glass). Foods such as margarine, eggs, chicken livers, salmon, sardines, herring, mackerel,swordfish, and fish oils (halibut and cod liver oils) all contain small amounts.Minerals and Bone Health
Although there are few food sources of Vitamin D, milk does contain significant amounts. (Fortified with Vitamin D, it contains 100 IUs per 250 ml glass). Foods such as margarine, eggs, chicken livers, salmon, sardines, herring, mackerel,swordfish, and fish oils (halibut and cod liver oils) all contain small amounts.Minerals and Bone Health