Sickle cell anemia
Sickle cell anemia is an inherited disease in which the Red Blood Cells get deformed to abnormal crescent shape.
Haemoglobin is a protein inside red blood cells that carries oxygen. Sickle cell anemia is caused by an abnormal type of hemoglobin called hemoglobin S. Hemoglobin S distorts the shape of red blood cells, especially when exposed to low oxygen levels. 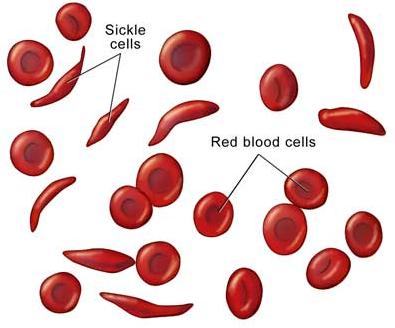 Hemoglobin S distorts the shape of red blood cells, especially when exposed to low oxygen levels. The distorted red blood cells are shaped like crescents or sickles. These fragile, sickle-shaped cells deliver less oxygen to the body’s tissues. They can also clog more easily in small blood vessels, and break into pieces that disrupt healthy blood flow.
Hemoglobin S distorts the shape of red blood cells, especially when exposed to low oxygen levels. The distorted red blood cells are shaped like crescents or sickles. These fragile, sickle-shaped cells deliver less oxygen to the body’s tissues. They can also clog more easily in small blood vessels, and break into pieces that disrupt healthy blood flow.
Sickle cell disease is much more common in people of African and Mediterranean descent. It is also seen in people from South and Central America, the Caribbean, and the Middle East. This disease is inherited from both parents. Someone who inherits the hemoglobin S gene from one parent and normal hemoglobin (A) from the other parent will have sickle cell trait. People with sickle cell trait do not have the symptoms of true sickle cell anemia.
In several sections of Africa, the prevalence of sickle cell trait (heterozygote) is as high as 30%.
The sickle cell disease gene is present in approximately 8% of black Americans. More than 2 million people in the United States, nearly all of them of African American ancestry, carry the sickle gene.
Sickle cell disease is present mostly in blacks. But is also found, with much less frequency, in eastern Mediterranean and Middle East populations.
The male-to-female ratio is 1:1.
It is a lifelong condition. It first manifests in the second half of the first year of life and persists for the entire lifespan.
Symptoms
The abnormality of the RBCs in this disease results in serious infections, chronic anemia, and damage to body organs. Each person can have different forms of complications from the disorder. Some children remain relatively healthy, while others are frequently hospitalized.
The presenting symptoms of this disease involve pain and anemia.
For the first 6 months of life, infants are protected largely by elevated levels of Hb F (fetal haemoglobin). Patients have painful episodes lasting for hours or days. These episodes affect bones of back, long bones and chest. Some patients have episodes every few years and some have many episodes every year.
The most common clinical picture during adult life is vasoocclusive crisis. The crisis begins suddenly, sometimes because of some infection or temperature change, such as an air-conditioned environment during a hot summer day. Severe deep pain is present in the long bones. The abdomen is affected with severe pain resembling acute abdomen. Pain may be accompanied by fever, malaise, and leukocytosis (high white cell count ). The crisis may last several hours to several days and terminate as abruptly as it began.
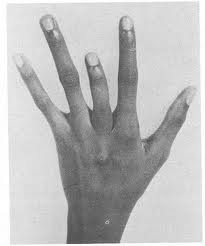
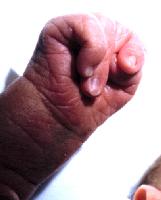
Shortened finger of African Adult male with sickle cell Disease
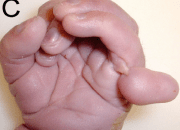
During childhood and adolescence, the disease is associated with growth retardation, delayed sexual maturation. The spleen enlarges in the latter part of the first year of life. The spleen may undergoes repeated infarction. Over time, the spleen becomes fibrotic and shrinks. Another problem occurring in infancy is hand-foot syndrome. This is a painful swelling of the dorsum of the hand and foot.
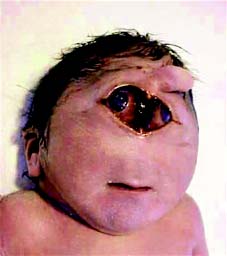
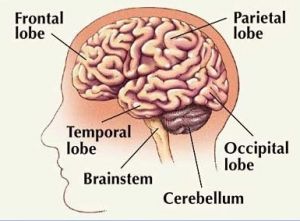
Central nervous system involvement may cause stroke with neurological deficit.
The heart is involved due to chronic anemia and and microinfarcts may damage it. Repeated Blood transfusion causes hemosiderin deposition in the myocardium.
Formation of Bile Stones due to chronic hemolysis with hyperbilirubinemia may cause Cholicystitis.
The lungs develop areas of microinfarction. The resulting areas that lack oxygenation aggravate the sickling process. Pulmonary hypertension may develop.
Leg ulcers are a chronic painful problem. They result from minor injury to the area around the malleoli.
Priapism (painful erection of penis) is a troubesome complication and tends to occur repeatedly. When it is prolonged, it may lead to impotence.
Spontaneous abortions may occur those who get pregnant.
Treatment
No cure is available for this disease.
The goals of treating sickle cell anemia are to relieve pain, prevent infections, organ damage, and strokes, and control other complications.
Children who are diagnosed with this disease need antibiotics to prevent infections and their parents need to be educated in managing the child.
Mild pain can be treated at home but for severe pain hospital treatment is needed. Dehydration and infections have to be managed. Oxygen therapy may be needed.
Hydroxyurea: can be used in patients of Sickle Cell Anaemia. It prompts the body to make fetal hemoglobin. Fetal hemoglobin, or hemoglobin F, is the type of hemoglobin that newborns have. In people who have sickle cell anemia, fetal hemoglobin helps prevent red blood cells from sickling and improves anemia. Given daily, hydroxyurea reduces how often painful sickle cell crises and acute chest syndrome occur. Many people taking hydroxyurea also need fewer blood transfusions and have fewer hospital visits.
Blood Transfusion is needed to treat anaemia and complications.
Infections can be a major complication of sickle cell anemia throughout life, but especially during childhood. Infection in children can be managed by giving daily doses of antibiotics.
All routine vaccinations (including a yearly flu shot), plus the pneumococcal vaccine is important.
Sickle cell anemia can damage the blood vessels in the eyes and the retinas. Regular eye checkup is needed.
Leg ulcers due to sickle cell anemia can be very painful. Ulcers can be treated with cleansing solutions and medicated creams or ointments.
Gallbladder surgery may be needed if the presence of gallstones leads to gallbladder disease.
Priapism (a painful erection in males) can be treated with fluids, medicines, or surgery.
Young children who have sickle cell anemia should have regular checkups with a hematologist.
New Treatments: Research on blood and marrow stem cell transplants, gene therapy, and new medicines for sickle cell anemia is ongoing. The hope is that these studies will provide better treatments for the disease.
New Medicines:
Decitabine, like hydroxyurea, this medicine prompts the body to make fetal hemoglobin.
Adenosine A2a receptor agonists, these medicines may reduce pain-related complications.
5-HMF. This natural compound binds to red blood cells and increases their oxygen. This helps prevent the red blood cells from sickling.