
TMT
TMT is the most widely used test in the diagnosis of ischemic heart disease. It involves recording the 12-lead ECG before, during, and after exercise on a treadmill.
The test consists of a standardized gradual incremental increase in external workload while the patient’s ECG, symptoms, and arm blood pressure are continuously being monitored. The test is discontinued upon evidence of chest discomfort, severe shortness of breath, dizziness, fatigue, ST-segment depression of greater than 0.2 mV (2 mm), a fall in systolic blood pressure exceeding 10 mmHg, or the development of a ventricular tachyarrhythmia.
This test helps to discover any relation between exercise and chest discomfort and the typical ECG signs of myocardial ischemia.
The ischemic ST-segment response is generally defined as flat depression of the ST segment of more than 0.1 mV below the baseline and lasting longer than 0.08 s. This type of depression is designated “square wave” or “plateau” and is flat or downsloping. Upsloping or junctional ST-segment changes are not considered characteristic of ischemia and do not constitute a positive test.
Although T-wave abnormalities, conduction disturbances, and ventricular arrhythmias that develop during exercise should be noted, they are also not diagnostic.
Negative exercise tests in which the target heart rate (85 percent of maximal heart rate for age and sex) is not achieved are considered to be nondiagnostic.
Overall, false-positive or negative results can occur in 15 percent of cases. However, a positive result on exercise indicates that the likelihood of CAD is 98 percent in males over 50 years of age with a history of typical angina pectoris who develop chest discomfort during the test. The likelihood decreases progressively and significantly if the patient has atypical or no chest pain. The incidence of false-positive tests is significantly increased in asymptomatic men under the age of 40 or in premenopausal women with no risk factors for premature atherosclerosis. It is also increased in patients taking cardioactive drugs such as digitalis and quinidine.
Since the overall sensitivity of exercise stress electrocardiography is only about 75 percent, a negative result does not exclude CAD, although it makes the likelihood of three-vessel or left main CAD extremely unlikely.
The physician should be present throughout the exercise test, and it is important to measure total duration of exercise, the times of the onset of ischemic ST-segment change and chest discomfort, The depth of the ST-segment depression and the time needed for recovery of these ECG changes are also important.
Because the risks of exercise testing are small but real estimated at one fatality and two nonfatal complications per 10,000 tests¾equipment for resuscitation should be available.
The normal response to exercise includes a progressive increase in heart rate and blood pressure. Failure of the blood pressure to increase or an actual decrease in blood pressure with signs of ischemia during the test is an important adverse prognostic sign, since it may reflect ischemia-induced global left ventricular dysfunction. The presence of pain or severe (>0.2 mV) ST-segment depression at a low workload and ST-segment depression that persists for more than 5 min after the termination of exercise increases the specificity of the test and suggests severe ischemic heart disease and a high risk of future adverse events.

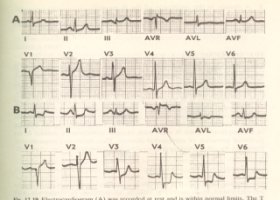
Lead V
4 at rest (
top) and after 4
1/
2 min of exercise (
bottom). There is 3 mm (0.3 mV) of horizontal ST-segment depression, indicating a positive test for ischemia.
Stress induced Electrocardiogram in a patient of Angina Pectoris
Illustration of typical exercise electrocardiographic (ECG) patterns at rest and at peak exertion. The patterns represent a gradient of worsening ECG response to myocardial ischemia.The first two tracings illustrate normal and rapid upsloping ST segments; both are normal responses to exercise.
Stress induced Electrocardiogram in a patient of Angina Pectoris
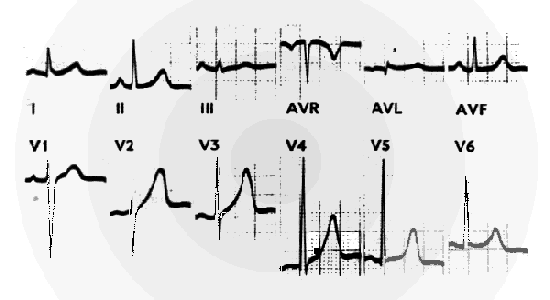
Normal Electrocardiogram
Angina Pectoris


 Lead V
Lead V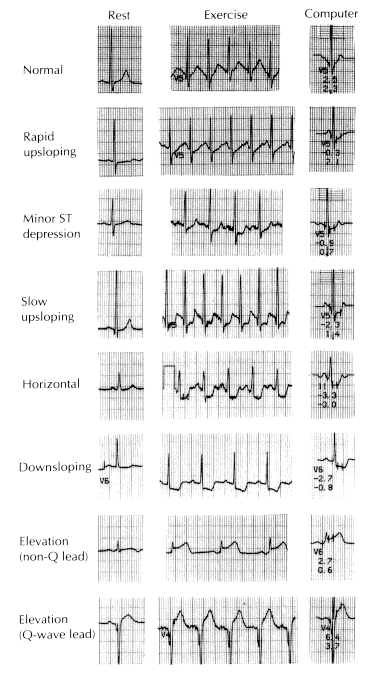

 Angina Pectoris is the name given to a clinical syndrome used to describe discomfort due to transient myocardial ischaemia. The underlying cause may be Coronary atheroma. Spasm of coronary artery may also be underlying cause.
Angina Pectoris is the name given to a clinical syndrome used to describe discomfort due to transient myocardial ischaemia. The underlying cause may be Coronary atheroma. Spasm of coronary artery may also be underlying cause.