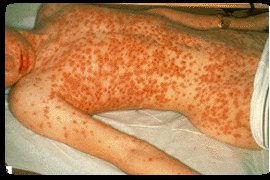
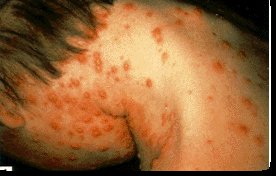
Cleft Lip & Palate
It is a sad experience for any parent to find its newborn child to have a birth defect of Cleft Lip and Palate. It is not only the parents, but also close relatives and friends, who get alarmed about the nature and the cause of the defect and worry about future development of the child. In general, birth defects could either involve internal organs, the external parts separately or both in varying combinations. Usually defects involving internal organs of the body are detected late in childhood either due to their effects on the child’s growth or due to incompatibility with life and thus do not have an immediate significant psychological stress. But birth defects like Cleft Lip and Palate are obvious immediately after the birth and these can cause more psychological problems to parents. Fortunately, with the modern surgical techniques available today, most of the deformities of Cleft Lip & Palate could be reconstituted to a near normal appearance and function.
Which other types of defects can be corrected with plastic surgery ?
The congenital defect coming under the scope of Plastic and Reconstructive surgery range from deformities of the External Ear, Facial Bones, Eyelids, Nose, Lips,
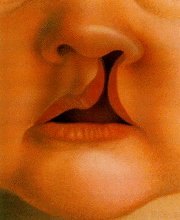
Cleft Lip before repair
Palate, Trunk, Extremities and Genitalia. Plastic Surgeons also use surgery for many types of cosmetic works.
Is it true that exposure to a Solar Eclipse during pregnancy can cause congenital deformities in the fetus?
It is a widely accepted and a popular myth, that watching of a solar eclipse by an expectant mother may lead to d evelopment of cleft lip in children, but fortunately, it does not have any scientific rationale. It is a fact, that parents often blame themselves for development of such birth defects in their children, which is totally wrong. In trying to find out the causes for such a calamity, they start believing in a number of unscientific theories like exposure to eclipse or God’s punishment etc. Often, under the belief that the God for some misdeed has punished them, they do not subject their children for surgical correction at proper age. Scientifically, it is extremely difficult to attribute any single factor responsible for any type of birth defect. Familial tendencies (hereditary), severe anemia during pregnancy, viral diseases like measles, typhoid etc. during early weeks of pregnancy, can be contributing factors. Drug addiction as well as excessive smoking of pregnant women may influence the development of the organs during the formative period i.e. 6 – 9 weeks of gestation. Also excessive use of antibiotics, painkillers, Vitamin A or sedatives, do have an effect on the fetus. However, it is difficult to pinpoint any single factor in a given case but these factors alone or in combination may lead to congenital defects.
What about the hereditary factor you had mentioned earlier?
Hereditary does play a significant role in development of certain congenital defects e.g. cleft lip and palate. If either of the parents or both, have this deformity, chances of

Cleft Lip after repair
their child developing a similar deformity is definitely more than otherwise. However, it is also not certain that a child will definitely inherit all birth defects of either of his / her parents.
Why is it that often-congenital defects not only affect the physical, but also the mental capacity of the child?
Congenital defects do have a great impact on a child’s physical, mental, psychological and personality development. By and large, most of these defects barring a few like hearing, vision or articulation of the speech, do not affect normal mental development or intelligence of the child. The feeling of not having something or looking different from others may sometimes make these children either more hostile or introverted in their personal life.
What is the Image building role of parents in such cases?
Parents should be well advised by their family doctor or attending physician to understand the exact nature of the birth defect and its implications, which would end up in influencing the development of personality complexes. For some times even after successful physical and functional correction of the defects, it is difficult for a child to revert back to normal behavior.
In order to avoid prolonged mental agony, is it advocated to resort to an Immediate Surgery for correction of this congenital defect?
It is not necessary that all defects are corrected immediately after birth, but a regular examination by the specialist doctor and monitoring the growth of the child, would be very helpful in over all rehabilitation of these children. Proper medical guidance and reassurance that the child would look as normal as otherwise and be able to perform most of the physical necessities effectively would defin itely restore the confidence of parents, thus influencing the child’s psychology in formative years of his life.
Is it possible that all these defects can be rectified with surgery?
Not all congenital defects need surgical procedures for their reconstitution. Quite a few of these defects are self-limiting and would cease to grow after a certain age. You will be surprised to know that many children with severe congenital deformities adapt to their deformities so well by natural development, that any surgical or external interference would hamper rather than help functioning of these children.
At what age is it advisable to undergo surgical correction?
Common and an ideal age for surgical correction of most of these congenital defects is preschool age, so as when the child leaves the protected atmosphere of his home and has to mix with unfamiliar faces, he is apparently normal both in appearance as well as in functioning. Some defects can be corrected in one stage; however, others may require a series of stages, depending upon the nature of the defect.
Which congenital defects in your opinion would require an early surgery? Deformities like cleft lip, cleft palate, club foot, extrophy of the urinary bladder, ano-rectal malformation, arterio-venous malformations etc., which either influence proper development of the child or hamper vital functions, are subjected to an early surgical procedure. On the other hand, defects like port wine stains, cavernous Hemangioma, polydactily, facial asymmetry, distal hypospadias etc. can be left untreated for years or to be operated upon after complete body growth.
Which is the most common congenital defect?
Cleft lip and palate is one of the commonest congenital defects. On average about 1 in 800 normal childbirth, has one of these deformities. It has been observed that cleft of the palate is found more in females than in males.
Is a cleft lip normally accompanied by a cleft palate?
The structural identification and formation of lip, palate and other organs begin sometimes between seven to nine weeks of gestation. Lip and palate develop independently embryologicaly, hence either of these defects could occur separately or in varying combinations. In case of cleft of lip, invariably upper lip is involved and may range from a small notch at the lower border to a complete cleft of the lip upto the base of the nose, either on one side or both. This may also extend up to teeth, jaw or even junction of eye and nose. Similarly the defect in the palate may be a small invisible hole in the mobile portion of the palate or split uvula to complete cleft of both the mobile (soft) and bony palate. This may also extend up to the jaws in continuity with the cleft of the lip or may occur alone. A mother would find it difficult to breast-feed her newborn infant, who has a cleft lip and palate.
How does she go about it?
Due to muscular deficiency associated with cleft lip and palate, the child cannot develop sufficient intra-oral pressure to suck the milk from the mother’s br east. A mother should understand this and either assist the child by manual pressure on the breast or feed the child with a spoon or even from a feeding bottle with a large nipple hole. It must be further understood that children born with a cleft lip and palate, have a tendency to swallow excessive air along with milk and burping them often is important.
At what age is it important for cleft lip and palate to be surgically operated?
The aim of surgery in these cases is to restore anatomical continuity of the affect part before their normal functioning utility. Surgical correction of the cleft lip deformity is done between the age of 3 months to 6 months. At few centers of the world including one in India, the cleft lip is corrected within 24 – 48 hours after the birth, so as to minimize the psychological impact on the parents and to take advantage of extra strong healing power at this age transferred to the neonate from his / her mother. In case of cleft of the palate, the ideal time for surgical correction is between 12-18 months before the child starts articulation of speech, as also the oral cavity becomes large enough to allow the surgeon to work inside. In some cases additional surgical correction may be required to improve the speech at around the age of 4 – 5 years.
In this modern high technology age, do all parents of children with such a congenital deformity of cleft lip and / or palate want to have this operation performed immediately?
You will be surprised to know that most of such children do not get proper medical attention or advise for surgical correction. Due to some unfounded myths, parents do not come forward requesting an immediate surgery and some do not bother at all. Recently, there was a case of Young lady of 62 years, who had this operation performed. Often unacceptable results are due to operation performed by an incompetent or unqualified surgeon and may require secondary corrections, when the child has reached adolescence.
Is there anything wrong in having this operation done at a later age?
When children with a cleft palate come for surgery at a later age, they pose one more problem of faulty speech and articulation habits. It would require postoperative treatment of a speech therapist to retrain the child for correct speech. If for some medical reasons, the child cannot be subjected to an early surgery, then a prosthetic obturator is recommended. For proper growth of the jaw and dental arches in these patients, orthodontic assistance is required and this treatment may continue till the age of 15-16 years.
What are other common congenital defects?
Deformities of extremities are one of the common congenital deformities. Congenital defects in Upper limbs vary from minor bending of fingers to a total absence of the limb. Commonly seen problems include joining of two or more fingers (Syndactily), presence of extra fingers or digit (Polydactily) or short fingers (Bradydactily), absence of thumb, index or more fingers etc. These may be associated with deformities of muscles and / or bones.
Can you explain the corrective surgery for such defects?
Supernumerary digit can be surgically removed. The joined fingers are usually separated at the age of 4 – 5 years, unless they hamper the normal growth of the adjoining finger. The absence of thumb can also be corrected either by transferring the great / second toe from the foot by Microvascular surgery or by repositioning the index finger in place of thumb. Most commonly seen congenital deformities of the external genital organs are hypospadias i.e. the urinary opening on the undersurface of the penis, epispadias – urinary opening on the dorsal surface of the penis or extrophy of the bladder. Genital organs may be poorly developed or totally rudimentary. Minor and rare deformities include torsion of penis, anterior location of scrotum, bifid penis or absence of vagina. Preschool age is usually best time to undertake and complete most of the Reconstructive Surgical steps. For extreme case e.g. Extrophy of the Urinary bladder, which requires a multi-stage correction, Reconstructive surgery is started at the age of 1- 1½ years.
Dr. Sanjeev Uppal
Plastic Surgeon
DMCH Ludhiana
133 D, Kichlu Nagar,
LUDHIANA 141001
suppal@satyam.net.in
Pregnant Women ~ need to know
 and in rainwater that collects in various containers (e.g. tyres, bottles, tanks, shallow wells, plastic bottles.)
and in rainwater that collects in various containers (e.g. tyres, bottles, tanks, shallow wells, plastic bottles.)

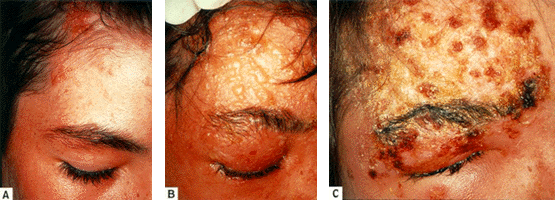




 febrile throughout the evolution of the rash and experiences considerable pain as the pustules grow and expand. Gradually, scabs form, which eventually separate, leaving pitted scars. In severe cases death usually occurs during the second week.
febrile throughout the evolution of the rash and experiences considerable pain as the pustules grow and expand. Gradually, scabs form, which eventually separate, leaving pitted scars. In severe cases death usually occurs during the second week.