Parkinson’s Disease
Is a chronic degenerative disorde. Its cause is still unknown.
Average age of onset: 57 years.
The disease was first identified in 1817.
Approximately 40,000 new American patients are diagnosed each year. In many cases the general “slowness” attributed to old age, may be an early symptom of PD.
People in rural areas are at higher risk of developing the disease than those in urban areas, perhaps because of exposure to pesticides, fungicides or herbicides through contaminated well water.
There is also a microorganism in the soil — Nocardia — that may damage dopaminergic neurons. Other high-risk environments include regions surrounding petroleum plants and pharmaceutical manufacturing plants.
Epidemiologists have noted that most PD patients have never smoked, and at least one study found a marked increase in the incidence of the disease among individuals with a history of mumps compared with those who never had mumps.
PD is not generally regarded as a genetic disease, although patients may inherit a predisposition. Some 14% of PD patients have one or more first-degree relatives who have the disease or a related disorder, compared to 5% of controls. Onset before age 40 is more often associated with a family history.
Low prevalence of Parkinsons’s disease among Indians is said to be due to the presence of some protective factors in the brain that inhibit the pathological changes leading to Parkinson’s disease.
Prevalence ratio:
North Americans: 280/100,000
Africans: 59/100,000
Chinese: 44/100,000
Indians: 19/100,000. Parsis living in India have the highest recorded prevalence rate of 328/100,000. (Parsis migrated to India from Persia now Iran.)
Parkinsonism is a syndrome consisting of three main components:
Tremor
Muscular Rigidity
Hypokinesis
(Hypokinesis is slowness in initiating & repeating voluntary movements)
Overall prevalence is about 1 / 1000 of the general population. There is a low prevalence of this disease among Indians. It is more common in elderly, the prevalence rising to 1% of those over 60 years.
Aetiology
The cause of the disease is not known. Genetic factors are not important in a typical case.
Environmental toxins may be a contributing factor.
Country areas frequently sprayed by herbicides show increased incidence of parkinsonism. Chemicals such as (MPTP) methyl-phenyl-tetrahydopyridine, paraquet have been implicated.
Clinical Features
Both sexes are affected equally. Onset of the disease is usually after 50 years. Very occasionally the symptoms may start in 3rd & 4th decade. Initially the classical symptoms may be absent. The disease may start as Tiredness, aching limbs, mental slowness, depression and small handwriting.
Face gives appearance of Expressionless face, Greasy skin, Fixed posture.
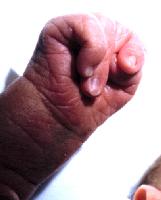
Tremor: Tremor at rest affecting one or both hands may be the first symptom. Tremor may also affect tongue, legs, mouth. Tremor may remain the only symptom for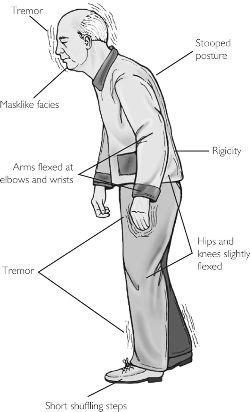 many years. Tremor is intermittent present at rest and when distracted. It diminishes on action.
many years. Tremor is intermittent present at rest and when distracted. It diminishes on action.
Hypokinesis: Difficulty in initiating rapid fine movements, slowness of gait, difficulty in tasks such as fastening buttons and writing.
Gait is typical – slow to start walking, shortened stride, rapid small steps, tendency to run, reduced arm swinging, and impaired balance on turning.
Rigidity of muscular tone: causes stiffness and flexed posture. Gradually the speech becomes softer and indistinct. Postural balance is disturbed because of impairment in the reflexes responsible for maintaining balance. Such patients are prone to falls. Rigidity is known as Cogwheel type in upper limbs and Plastic lead pipe type in the lower limbs.
Features of parkinsonism may be unilateral in the beginning but gradually they become bilateral. Muscle strength and reflexes remains normal. Facial reflexes are enhanced. Tapping of the forehead causes rapid blinking known as Glabellar tap sign. Intellectual faculties are not markedly affected. Some patients may get depressed and there may be some cognitive impairment as the disease advances.
Management
Drug therapy
L-DOPA
The rationale for using L-DOPA is that the enzyme step converting the precursor DOPA to Dopamine is dependent on the concentration of the substrate. Although in parkinsonism the number of dopamine releasing terminals in the striatum is diminished it is possible to overdrive the remaining neurons to produce more dopamine by administering DOPA.
More than 90% of the orally taken L-DOPA is decarboxylated in the gastrointestinal tract to dopamine and only a small amount reaches the brain. If L-DOPA is used alone there is high incidence of side effects such as nausea, vomiting, vasodilatation. This problem is solved by giving a peripherally acting decarboxylase inhibitor. This combination therapy permits use of low dose of L-DOPA.
L-DOPA + Carbidopa
L-DOPA + Benserazide
The combination should be started with low dose and gradually increased. Tremor, Rigidity and hypokynesis are improved.
With the progression of the disease there is loss of capacity to store dopamine. Late deterioration in response to L-DOPA therapy occurs after 3-5 years in 1/3 to 1/2 of patients.
Selegiline and Bromocriptine may be helpful at this stage.
Bromocriptine is preferably used as a low dose combination with L-DOPA. Especially in young patients who need treatment for many years.
Surgery
Stereotactic thalamotomy is occasionally performed in patients with severe unilateral tremors not responding to drugs.
Implantation of Fetal mid brain or Adrenal cells into the basal ganglion in parkinsonian patients has been tried.
Physiotherapy and Speech therapy is needed to reduce rigidity and to correct posture.
Other drug:
Benxhexol 1-5 mg tid
Orphenadrine 50-100 mg tid
Have useful effect on tremor and rigidity. Do not help hypokynesis. They should be used in early stage of the disease when hypokynesis is not a problem.
Side effects: dryness of mouth, blurring of vision, difficulty in micturation and constipation.
Amantidine 100mg bid or tid
It has mild short lived action on hypokinesis.
Side effects: oedema, confusion, seizures.
Ropirinol – Requip – ( SmithKline Beecham )
Pramipexole – Mirapex – ( Pharmacia & Upjohn )
Tolcapone – Tasmar – ( Roche )
Disorders that may mimic Parkinsons disease
Benign essential or familial tremor, a slowly progressive condition that usually develops in the fourth and fifth decades.
Symptoms include a tremulous voice and shaky hands and/or head (the head may bob side to side or up and down).
The typical parkinsonian rigidity, stiffness and bradykinesia do not occur.
Hyperthyroidism can also cause tremor.
Other more serious conditions that may mimic PD include Progressive Supranuclear Palsy, Shy-Drager Syndrome.
Parkinson’s Gene
Parkinson’s Disease – Genetic & Environmental etiology
Coffee and Parkinson’s disease









 many years. Tremor is intermittent present at rest and when distracted. It diminishes on action.
many years. Tremor is intermittent present at rest and when distracted. It diminishes on action.