Hyperhydrosis |
| Sweating is a natural process by which body regulates an individual’s body temperature. The system that regulates all this is known as Sympathetic Nervous system.In approximately 1% of the population this system is working at a higher level and thus this problem of Hyperhydrosis.
We divide hyperhydrosis into Two types: Idiopathic – of which the cause is unknown and the second one is secondary to some disease process. Causes of Secondary Hyperhydrosis
Idiopathic Hyperhydrosis This is a far more frequent condition than secondary hyperhydrosis and is generally, localized in one or several locations of the body (most often hands, feet, armpits or a combination of them). It usually starts during childhood or adolescence and persists all life. Nervousness and anxiety can elicit or aggravate sweating, but psychological/psychiatric disturbances are only rarely the cause of the disorder. Sweating can appear suddenly or manifest itself more continuously. Treatment In patients with primary hyperhidrosis or for symptomatic treatment of heavy sweating in patients with secondary hyperhidrosis, not treatable otherwise, the following methods have been adopted. Anti Perspirants Aluminium chloride (20-25%) in 70-90% alcohol, applied in the evening Alternate days. This method consists in applying low intensity electric current (15-18 mA), supplied by a D/C generator, to the palms and/or soles immersed in an electrolyte solution. It is difficult to apply in axillary, and impossible to use in diffuse hyperhidrosis of the face or the trunk/thigh region. Drugs There are no specific drugs available against profuse sweating. Sedatives or Anticholinergics are often tried. Anticholinergics show too many side effects. Surgery
Patients with axillary hyperhidrosis who are unresponsive to medical therapy can be effectively treated by excision of the axillary sweat glands.
The principle of sympathectomy is to interrupt the nerve tracks which transmit the signals to the sweat glands. The endoscopic technique is very safe, if performed by a surgeon experienced in this type of procedure, leads to definitive cure in nearly 100% of patients, leaving only a minimal scar in the armpit. Individuals with combined hyperhydrosis of the palms and soles have a good chance to improve the sweating of their feet after an operation aiming to suppress sweating of the hands. Isolated plantar hyperhydrosis can, however, only cured by Lumbar Sympathectomy, an open abdominal procedure. Diffuse hyperhydrosis of the trunk or general sweating of the whole body cannot be treated by surgery. OTHER TREATMENT METHODS
A family of toxins produced by bacteria known as Clostridium botulinum. This toxin is one of the most lethal poisons known, interfering with the effect of the transmitter substance acetylcholine at the synapses (the contact point of a nerve ending with another nerve cell or a muscle) and leading to progressive paralysis of all muscles in the body, including the respiratory muscles. |
Category Archives: Diseases & Conditions
HIV ~ Human Immunodeficiency Virus
|
Human Immunodeficiency Virus |
The Human Immunodeficiency Virus (HIV) is a deadly virus. Once you are infected with this virus you are sooner or later going to develop AIDS ‘Aquired Immunodeficiency syndrome’. There is at present no cure for this disease. It is spread from one person to another via blood, semen, and vaginal fluids. Once you become infected, the virus attacks and gradually weakens your body’s Immune System which is the defence mechanism against infections which our body is exposed at every minute of our life. Thus this reduced defence system of our body makes it possible for unusual diseases and cancers to take hold in our body.
HIV infection and AIDS are caused by infection with the human immunodeficiency virus (HIV). HIV infects CD4+ cells, also known as T-helper cells or Helper T Lymphocytes, which are part of the body’s immune system. There are mainly two types of HIV virus, HIV-1 and HIV-2. HIV-1 causes most of the infection all over the world.
How the disease is spread
HIV is spread when blood, semen, or vaginal fluids from an infected person enter another person’s body, usually in one of the following ways:
Sexual Contact: any type of sexual contact – anal, vagina, or oral.
Drug addicts sharing needles.
Tattooing and body piercing by unsterilized needles. Getting injected by unsterilized needles by quacks (especially in the underdeveloped countries.)
Accidental needle pricks to health workers or doctors.
Unsafe Blood or blood products.
Born to HIV positive mother. Pregnant female can transmit the virus to the newborn during pregnancy or during delivery or when she feeds her baby breast milk.
After years of scrutiny, there is no evidence that HIV is transmitted by casual contact or that the virus can be spread by insects, such as by a mosquito bite.
AIDS is diagnosed when an HIV-infected person has —
- A CD4+ cell count below 200 cells per microliter of blood.
- Specific opportunistic infections and/or cancers
About 60% of HIV-positive adults who do not receive treatment develop AIDS after 12 or 13 years .This time period is too variable. Many with positive HIV develop opportunistic infections early and succumb to such infections.
Homosexuals, those who inject drugs and those with promiscuous lifestyle form a big part of HIV infections. Those visiting sex workers are at a very high risk. Truck drivers especially in the developing countries like India are a major part of infected population and are taking a big part in the spread of this infection back to their family when they happen to visit home.
| The risk of an HIV-positive woman spreading the virus to her baby can be greatly reduced if the mother takes a drug called zidovudine (ZDV) during pregnancy and if she does not breast-feed her baby. The baby should also receive ZDV after it is born. |
| Herpes simplex virus type 2 infection was one of the strongest risk factors for HIV acquisition among men who have sex with men. |
|
Pathogenesis |
| The Human immunodeficiency virus is made up of Genetic material, Chemicals and a coating. The Genetic material is RNA and the Chemicals are enzymes which help the virus enter and use other cells to make copies of itself.HIV mainly infects white blood cells called T-lymphocyte cells (T-cells). The virus infects a T-cell by attaching to a protein on the cell’s surface called CD4+. Not all T-cells have this protein. The ones that do are called CD4+ cells, T4 cells, or T-helper cells.After binding with the CD4+ cell, the virus enters the cell and, using an enzyme called reverse transcriptase, merges its RNA with the cell’s genetic material (DNA). This causes the DNA in the CD4+ cell to make copies of HIV (replication). Another enzyme called protease helps the new viruses to form. The new viruses then “bud” off the infected cells into the body, where they infect more CD4+ cells.The presence of the virus causes a person’s immune system to react by attacking the virus itself and any HIV-infected cells. This process results to formation of antibodies . A person is said to be HIV-positive if antibodies to the virus are detected by tests, indicating infection.As HIV-infected CD4+ cells are destroyed or impaired, the person’s immune system becomes less and less effective at fighting infection and disease. The person is said to be “immunocompromised” or “immunodeficient.” Such people are more likely to develop unusual diseases called Opportunistic infections that they would not get if their immune systems were healthy.As the number of CD4+ cells decreases, the person is more likely to get sick and have more serious illnesses. When this is the case, a person is usually diagnosed with acquired immunodeficiency syndrome (AIDS). |
In a healthy person, the normal range of certain white blood cells called T4 lymphocyte cells (helper cells) is usually between 600 and 1200 (T4) cells per cubic millimeter (cells/mm3). (The range depends on the test used.) When human immunodeficiency virus (HIV) enters the bloodstream, it primarily infects T4 cells. Asymptomatic individuals infected with HIV usually have a lower than normal T4 cell count, and people with AIDS generally have between 0 and 500 T4 cells/mm3. The number of T8 lymphocyte cells (suppressor cells) in an HIV-infected person usually stays about the same. Because the number of T4 cells is low, the total T-cell count is lower than normal, and the T4/T8 cell ratio is lower than the usual 2 to 1 ratio.
HIV infection not only reduces the number of T4 cells, it can also impair a T4 cell’s functioning. HIV-infected individuals with very low T4 cell counts tend to have more serious infections. Therefore, regular immunologic tests to determine T4, T8, and total T-cell counts can be an important element in monitoring the health of an HIV-infected person.
Two types of HIV have been identified to date: HIV-1 and HIV-2. HIV-1 is the predominant HIV type in the United States and throughout the world. HIV-2 is primarily found in West Africa.
Origin of HIV Virus
HIV-1 originated in non-human primates, probably chimpanzees. The origin of HIV-2 has been identified as being another monkey species, the sooty mangabey (Cercocebus atys). |
|
Clinical Features & Symptoms |
A wide variety of symptoms can be expected in patients infected with HIV. Combination of various indicators can help in diagnosing this disease. A high degree of suspicion can help in diagnosing many patients in their early stage.
- Fatigue
- Weight loss
- Fevers
- Night sweats
- Swollen lymph nodes in neck, armpits, and groin
- Sinus fullness and drainage
- Pain when swallowing
- Mouth sores
- Dry cough
- Shortness of breath
- Diarrhoea or other bowel changes
- Personality changes
- Difficulty concentrating
- Confusion
- Tingling, numbness, and weakness in the limbs
- Dry skin
- Nail changes
- Recurrent Herpes Simplex
HIV infection may be suspected when a woman has the following:
- Recurrent vaginal yeast infections (more than 3 infections per year.)
- Recurrent Pelvic Inflammatory disease.
- Abnormal Pap test
HIV may be suspected in a child who has the following:
- Persistent yeast infection of the mouth (thrush)
- Recurrent bacterial infections
- Delays in growth or development
- Swollen lymph nodes in neck, armpits, and groin
- Enlargement of the liver and spleen
Almost all of these symptoms can be caused by other illnesses too.
AIDS is diagnosed when an HIV-infected person has a CD4+ cell count below 200 cells per microliter of blood and specific opportunistic infections and/or cancers.
Primary Infection
The initial infection with HIV is a subclinical type of infection and may not be of much consequence. A small part of the infected may develop within 2-3 weeks Rash, Fever and Lymphadenopathy. Some get pharyngitis, erythematous maculopapular rash, arthralgia, myalgia, retro-orbital headache, malaise, diarrhoea and vomiting. Opportunistic infections are not seen at this stage.
A large majority remain without any symptom. After a long incubation period varying from 1 to 12 years (usually 5-7 years) majority of the HIV infected develop frank clinical problems. The clinical picture is also too variable and depends from patient’s level of immune system.
Many develop serious opportunistic infections especially Pn.carrini pneumonia and Kaposi’s sarcoma. Kaposi’s sarcoma is a cancer of the walls of the blood vessels or lymphatic system. It usually appears as pink-to-purple spots on the skin. It can also occur internally. Kaposi’s sarcoma can be fatal if it develops in certain sites such as the lungs.
sarcoma. Kaposi’s sarcoma is a cancer of the walls of the blood vessels or lymphatic system. It usually appears as pink-to-purple spots on the skin. It can also occur internally. Kaposi’s sarcoma can be fatal if it develops in certain sites such as the lungs.
Some HIV infected develop symptoms like diarrhoea, weight loss, candidiasis, fever and leucopaenia.
Brain involvement occurs in a large number of infected patients. This can be in the form of Dementia, Psychosis, Encephalitis, Multiple cerebral abscess, Cerebral toxoplasmosis, Herpes encephalitis, Cerebral lymphomas, Kaposi’s sarcoma, Stroke, Mylopathy, Neuropathy, Fungal infection.
encephalitis, Cerebral lymphomas, Kaposi’s sarcoma, Stroke, Mylopathy, Neuropathy, Fungal infection.
The diverse nature of the neurological complications underlines the importance of considering HIV infection in any neurological patient.
In Africa, majority of patients present with severe weight loss. Multiple parasite infection is very common in African patients and thus diarrhoea is also very common.
Thrombocytopenic purpura may be isolated manifestation of HIV infection.
|
|
|
Opportunistic Infections in AIDS |
The HIV virus causes a chronic infection that leads to profound immuno-suppression. The course of the infection may vary with some individuals developing immunodeficiency with 2 to 3 years and others remaining AIDS free for 10-15 years.
Eventually the infected individual develops Early symptomatic HIV, which progresses to AIDS with associated opportunistic infections and malignancies.
The manifestations of infections in AIDS patients depend on the level of immunity, which is reflected by the CD4+ T cell count. The majority of the infections occur when the CD4 cell count falls below 500 cells/mm³. These include pneumoccocal and other pneumonia, pulmonary tuberculosis, Herpes Zoster, candidisis, Kaposi’s sarcoma, cryptosporidiosis, Oral hairy leukoplakia.
Levels lower than 200 cells/mm³ are associated with P.carini pneumonia, Toxoplasmosis, miliary and extra pulmonary tuberculosis.
Levels lower than 50 cells/mm³ is associated with disseminated CMV and Mycobacterium avium complex.
Early symptomatic HIV disease
At this stage symptoms including fever, unexplained weight loss, recurrent diarrhoea, fatigue and headache. Coetaneous manifestations like seborrheic dermatitis, folliculitis, recurrent herpes simplex infections oral hairy leukoplakia may occur. During this period the CD4 T-cells count continues to come down. Usually anti retroviral therapy is started at this stage.
Opportunistic Infections are important part of the HIV disease process. It is common to find AIDS patients with multiple OIs. These OIs result in more rapid decline in CD4 T-cell count than the decline resulting from HIV disease itself. Thus effective therapy is required to treat and prevent this infection. The incidence and type of OIs in HIV patients is directly related to the CD4 count in that individual.
Common OIs are Tuberculosis both pulmonary and extra-pulmonary, Oropharyngeal candidiasis, Herpes zoster, Herpes simplex, Toxoplasmosis, Cryptococcal Meningitis, Pneumocystitis carini pneumonia, Cytomegalovirus retinitis, Cryptosporidial diarrhoea.
Tuberculosis
It ranks one of the most common opportunistic infections. TB can occur in early stage HIV patients with CD4 cell count < 300 cells/mm³. Clinical presentation is usually similar to that in non-HIV patients. Typical symptoms include productive cough of several week’s duration, fever, weight loss, night sweats and haemoptysis.
In patients with advanced HIV disease extra-pulmonary disease is more common. Disseminated disease with involvement of bone marrow, bone, urinary and gastrointestinal tract, liver, regional lymph nodes, and central nervous system is common. Tuberculosis in HIV patients may show atypical findings in the chest x-ray, negative tuberculin reaction, and extra pulmonary lesions.
Management of HIV related tuberculosis is complicated as there is significant interaction between antiretroviral therapy and standard anti-TB medication.
Mycobacterium Avium Complex (MAC)
MAC consists of atypical bacteria like Mycobacterium avium, M. intracellulare, and some other strains commonly seen in AIDS patients in western hemisphere, but is rarely seen in Indian subcontinent. The diagnosis is based on recovery of MAC in culture of blood and bone marrow. Treatment is with Clarythromycin 500 mg twice daily + Ethambutol 15 mg / kg/day and to continue the treatment for life. The treatment may be discontinued if the CD4 count becomes > 100 cells.
FUNGAL INFECTIONS
Fungal Infections are one of the commonest causes of mortality and morbidity in HIV patients. Majority of the patients go downhill because of these infections and they prove to be the cause of death. Candidiasis is one of the commonest fungal infections seen in HIV patients. Other fungal infection is Cryptococcal meningitis, Histoplasmposis, and Pneumocystis carinii pneumonia (PCP)
Candidiasis
Oral candidiasis is extremely common in AIDS patients. The most common pathogen is Candidia albicans. Other pathogens are C.glabrata, C.krusei and C.parapsilosis. Most commonly the presentation is Oropharyngeal Candidiasis – in this both the mouth cavity and the pharynx is involved. It generally presents as burning pain, altered taste sensation and difficulty in swallowing liquids and solids. Painless white patches are found on the tongue, gums, buccal mucosa, tonsils and pharynx. Oesophageal candidiasis is diagnosed when dysphagia is present with thrush.
Anti fungal therapy has to be given.
- Mild Oral candidiasis responds to topical application of clotrimazole or nystatin.
- Most of the patients need to be given Fluconazole 200mg on the first day followed by 100mg once daily for 7-14 days.
- Alternatively Itraconazole 100mg daily for 7-14 days may be used.
Cryptococcosis
The most common manifestation fo cryptococcosis is meningitis. It is caused by Cryptoccocus neoformans. Common presenting symptoms are severe headache, fever, progressive malaise, nausea, fatigue, loss of appetite and altered mental status. Typical clinical signs of meningitis may not be seen in such patients.
It is treated with Amphotericin B and Flucytosine, such patients may need to be put on lifelong oral fluconazole.
Pneumocystis carinii pneumonia (PCP)
This infection in HIV patients presents as Fever tachypnoea and dry cough. Trimethoprim-sulphamethoxazole orally is effective for this condition. Its dose is 2 tab given 8 hrly for 2-3 wks. Such patients have to be put on prophylaxis against PCP with one tab of this medication every day.
VIRAL INFECTIONS
Common viral infection in HIV patients are Herpes zoster, Genital herpes, Herpes labialis and CMV retinitis.
Most of the episodes of genital and herpes labialis are thought to be reactivation of the latent infection. Treatment for this includes Acyclovir 200-400 mg 5 times daily for 10-14 days. For prevention continuous therapy may have to be given.
Primary infection with varicella zoster virus leads to severe chicken pox in HIV patients. Herpes zoster tends to occur within months of the primary infection rather than years after the primary infection in case of non-HIV individuals. Oral acyclovir is the preferred therapy.
Cytomegalovirus disease
Retinitis is the most common manifestation of the CMV infection in the HIV patients. The symptoms include light flashes, floaters, loss of central and peripheral visual fields and blurred vision. Ganciclovir is used in this condition.
PROTOZOAN INFECTIONS
Toxoplasmosis is caused by toxoplasma gondii. Most common manifestation is encephalitis. It presents with severe headache, focal neurological deficits, fever, and confusion. Diagnosis is made with CNS masses on CT or MRI scans and positive toxoplasma serology.
Treatment includes Sulphadiazine, pyrimethamine, folic acid.
AIDS ASSOCIATED DIARRHEA
Diarrhoea is the most common Gastro intestinal complication in people who are infected with HIV. It can be caused by bacteria like salmonella, shigella, camphylobacter. Parasites like cryptosporidium, isospora, giardia, microsporidia. Mycobacterium tuberculosis, MAC. Viral – cytomegalovirus. Diarrhoea may also occur due to side effects of the drugs like protease inhibitors.
|
Investigations |
Two tests are used to diagnose HIV infection. They detect antibodies to HIV.
- ELISA ( Enzyme-linked immunosorbent assay. If it is negative, no further tests are needed.
- Western Blot Assay. It is used to confirm a positive ELISA test.
It can take up to 6 months, usually 3 months from the time of exposure to HIV until antibodies can be detected. During this period the person can spread infection to others.
HIV infection is diagnosed only after 2 or more positive ELISA tests are confirmed by a positive Western blot assay.
Laboratory tests for detecting HIV infection are of three types
- Screening tests
- Supplemental tests
- Confirmatory tests
Screening tests: are designed to detect Antibodies against HIV.
They are of three types.
ELISA – enzyme linked immunosorbent assay test
Rapid Tests
Simple Tests
ELISA technology is based on antigen-antibody and enzyme substrate reactions.
Rapid Tests – Dot Blot and Latex Agglutination Tests
Simple Tests – Particle Agglutination tests.
Both Simple and Rapid Tests do not need costly equipments.Strategies employed for HIV screening.
Strategy I
Used for blood transfusion safety. The serum of the donor is tested by one of the techniques E/R/S (ELISA, Rapid, Simple Tests) If reactive it is taken as Positive and if non reactive it is taken as negative.
Strategy II
If the serum is reactive with one of the E/R/S it is tested with a second E/R/S based on a different antigen or on different test principle. If the second test is reactive it is reported as positive. If it turns out to be non reactive it is reported as negative.
Strategy III
If the serum sample is found to be reactive with two E/R/S tests, it is retested with a third E/R/S, again with a different antigen or a different test principle.
Supplemental Tests – Western Blot test, Immunofluorescent tests. These are used to validate results obtained by the screening tests. Western Blot test is highly sensitive test. Like ELISA it may not be positive in the initial 3-4 wks of infection.
Confirmatory Tests – aim at demonstration of Viral Antigen(P24), isolation of HIV and detection of viral nucleic acid. These are done in the reference centres and are time consuming and very costly. The confirmatory tests can diagnose HIV infection even during the initial two to three weeks – the window period, in which both the screening and the supplemental tests fail to diagnose the infection.
Elisa (Enzyme Linked Immunosorbent Assays)
ELISA is the most commonly used test to screen for HIV infection. It detects antibodies to HIV. ELISA may not be sensitive during the initial 3-4 wks of infection because the HIV specific antibodies become positive about 22 to 27 days after acute infection.
False positive tests may occur in multiparous women, recent recipients of Influenza or Hepatitis B vaccines or multiple transfusions, those with haematological malignancies, multiple myeloma, primary biliary cirrhrosis or alcoholic hepatitis.
False negative ELISA occurs in very early or late in the course of HIV disease when antibody production is low.
Rapid progressors
About 5% to 10% of people who are infected with HIV are “rapid progressors.” They develop AIDS within about 3 years if they do not receive treatment.
Nonprogressors and HIV-resistant people
Some people never become infected with HIV despite years of exposure to the virus (for example, they may have repeated, unprotected sex with an infected person). These people are said to be HIV-resistant.
| At least 5% of HIV-positive people are described as “nonprogressors.” These people have lived with the infection for 10 to 15 years but they have stayed healthy and do not have declining CD4+ cell counts. |
Genital Warts & HPV
|
Genital Warts & HPV |
Genital warts are caused by Human Papilloma Virus (HPV). They were long considered inconvenient but benign conditions. Most genital warts are caused by HPV types 6 and 11, which are rarely if ever associated with invasive cancers. However, other strains of HPV (High Risk types) e.g., types 16, 18, 31, 33, 35, 39, 45, 52, 55, 56, and 58 are implicated in the development of moderate to severe squamous dysplasia and of overt cancer of the cervix, anus, vulva, vagina, and penis.
Human papillomaviruses (HPVs) selectively infect the epithelium of the skin and mucous membranes. These infections may be asymptomatic (without any problem), produce warts, or be associated with a variety of benign and malignant diseases.
The incubation period of HPV disease is usually 3 to 4 months, with a range of 1 month to 2 years.
- There are many different types of genital HPV.
- Only certain types of HPV are linked with cervical cancer. These are usually called “high-risk” types.
- The types of HPV that cause raised external genital warts are not linked with cancer. These are called “low-risk” types.
- These wart-types of HPV usually are not usually found on a female’s cervix, and therefore, are not going to carry any risk of cancer.
- It is common for a person to be exposed and have more than one type of HPV, including several “high-risk” types. Yet, most women do not develop cervical cancer.
- Cervical cancer usually takes years to develop.
- Most of the time, men will not have any symptoms or health risks such as cancer with the “high-risk” types of HPV. It is the female’s cervix that needs to be monitored.
Other types of warts
Common warts (verruca vulgaris) most prevalent among young children.
Plantar warts (verruca plantaris) are also widely prevalent; they occur most often among adolescents and young adults.
Condyloma acuminatum (which manifests as anogenital warts) is one of the most common sexually transmitted diseases.
Common warts usually occur on the hands as flesh-colour to brown, hyperkeratotic papules. Plantar warts may be quite painful. Flat warts ( verruca plana) are most common among children and occur on the face, neck, chest, and flexor surfaces of the forearms and legs.
Anogenital warts develop on the skin and mucosal surfaces of the external genitalia and perianal areas. In men, warts are found most frequently at the frenum or coronal sulcus but may affect any part of the penis. They occur commonly at the urethral meatus and may extend proximally. Perianal warts are common among homosexual men but develop in heterosexual men as well. In women, warts appear first at the posterior introitus and adjacent labia. They then spread to other parts of the vulva and commonly involve the vagina and cervix. These lesions may be present without external warts.
The anogenital warts may be confused with many other types of diseases like condylomata lata of secondary syphilis, molluscum contagiosum and a variety of benign and malignant mucocutaneous cancers.
Infections involving the Respiratory system in young children may be life-threatening and presents as hoarseness, stridor, or respiratory distress. The disease in adults is usually mild.
The complications of warts include itching and occasionally bleeding. In rare cases warts become secondarily infected with bacteria or fungi. Large masses of warts may cause mechanical problems, such as obstruction of the birth canal. Dysplasias of the uterine cervix are generally asymptomatic until frank carcinoma develops.
Treatment
Currently available modes of treatment are not completely effective. Many lesions resolve spontaneously. Frequently used therapies include cryosurgery, application of caustic agents, electrodesiccation, surgical excision, and ablation with a laser. Topical antimetabolites such as 5-fluorouracil also have been used. Both failure and recurrence have been well documented with all of these methods of treatment. Cryosurgery is the initial treatment of choice for condyloma acuminatum. Topically applied podophyllum preparations as well as podofilox may also be used. Various interferon preparations have been employed with modest success in the treatment of respiratory papillomatosis and condyloma acuminatum.
Genital Warts
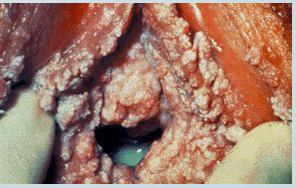 |
Typical papilliferous warts (condyloma acuminata) affecting the vulva and vagina. |
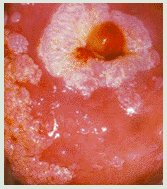 |
Typical papilliferous warts (condyloma acuminata) affecting the cervix. |
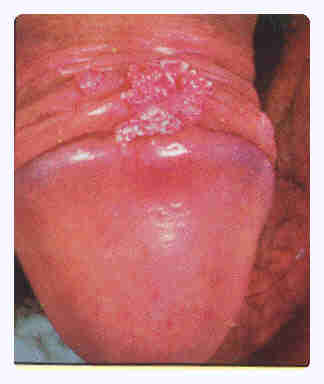 |
Veneral Warts of Penis |
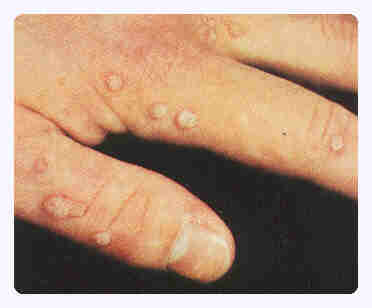 |
Common Warts |
Human Genome
Human Genome
|
On Monday 26 June 2000, after more than a decade of effort, a working draft of the human genome was presented to the humanity. This day would be remembered as the day when humankind learned about the set of genetic instructions which governs the assembly and fuction of human beings.
The scale of this triumph of biological science is awesome.
- The 24 different human chromosomes may be too small for the eye to see, but each set contains 3.1 billion base pairs: a code written in 3.1 billion “letters”. This amount of data is equivalent to the contents of 200 telephone directories, each 500 pages long. It has been estimated that it would take over nine years to read aloud this data.
- If all the DNA in the human body were put end to end, it would reach to the sun and back more than 600 times.
- There are 20 different building blocks (amino acids ) used in an array of combinations to produce proteins as different as keratin in the hair and haemoglobin in the blood.
- The vast majority of the DNA (97 % ) in human genome has no known function.
- Between humans the DNA differs by only 0.2 %.
- Human DNA is 98 % identical to chimpanzee.
- Scientists estimate that there are 300,000 spots in the human genetic code where individual differences can exist.
Reading Human genome code took the combined efforts of thousands of researchers, and countless hours of work by hundreds of state-of-the-art robotic sequencing machines humming quietly around the clock in pristine laboratories. Each machine prepares DNA samples, runs them through electrophoresis gels, and reads off the results into a database, only requiring the help of a human once every 24 hours.
The public Human Genome Project took blood and sperm samples from a dozen anonymous donors and combined them. The project’s commercial rival, Celera Genomics, put an ad in The Washington Post, selected 30 men and women from a variety of ethnic backgrounds and used six of them.
Estimated number of genes:
Humans & mice – 60,000 to 100,000
Roundworm – 19,000
Yeast – 6,000
| October 16, 2002 |
| Researchers have come up with some new findings. That the genome has revealed that the human chromosome carries only about 30,000 genes, twice the number of a fruit fly, 10,000 more than a roundworm, and only a few hundred more than a mouse. Originally scientists expected as many as 140,000, which means the question of how genes actually work is now an even bigger mystery. The genome also reveals that many human genes originate from microbes. This raises questions about human evolution. |
In future:
- Doctors may treat you for conditions such as cancer and heart disease even before they appear. There may be fundamental shift towards preventive medicine.
- A routine check-up in future will perhaps involve giving a sample of blood from which your DNA will be extracted and screened to determine your risk of developing various diseases.
- We already know the genes that cause many rare, single-gene disorders, but in future you could be screened for common diseases that appear in adulthood, such as type II diabetes, heart disease and cancer, and perhaps even complex mental disorders such as schizophrenia and depression. Because these diseases have many contributory factors, both genetic and environmental, the test results will give a percentage risk rather than a definite yes or no.
- Doctors may also use gene screening to discover which drugs best suit you. Our genes determine whether different drugs will work well or cause side effects. For example, Alzheimer’s patients with a gene variant called ApoE 4 are much less likely to benefit from a drug called tacrine than other patients.
- The insurance agencies making use of genetic information is a possibility.
| A single gene may play a role in the development of cancer and a number of age-related diseases, including arthritis, hardening of the arteries and Alzheimer’s disease, according to new study findings. |
Gene Therapy Genetic disorders Genome Sequencing helps diagnosing rare disorder
Gene Therapy
Gene Therapy
|
Gene therapy is a newer approach to treating diseases based on modifying a person’s genes toward a therapeutic goal. Gene therapy has been targeted towards treating lethal and disabling diseases. It also has potential of preventing diseases. This method of treatment is still in its infancy.
It can be said that the gene that we inherit from our parents influence practically every disease. A composite of approximately 150,000 individual genes constitutes a human being. Several years ago, an international effort was launched to identify every single human gene. This effort, called the Human Genome Project. Variation in the structure of a person’s genes collectively helps define us as individuals such as how tall we are to what color our eyes are supposed to have. Some of this genetic ‘miscalculations’ unfortunately leads to the development of disease. The genetics of many diseases are passed from one generation to the next by inheriting a single gene. An example is Huntingdon’s disease. Many other diseases and traits are influenced by a collection of genes.
The premise of gene therapy is to treat the disease at its root. There are two types of Gene Theapy. Somatic Gene Therapy and Germline Gene Therapy.
Somatic gene therapy involves the manipulation of gene expression in cells that will be corrective to the patient but not inherited to the next generation.
Germline gene therapy, this involves the genetic modification of germ cells that will pass the change on to the next generation.
It is the Somatic Gene therapy that is being mainly investigated throughout the world. The work on Germline gene therapy is restricted due to technical and ethical reasons.
To deliver genetic material to the appropriate cells of the patient in a way that is specific, efficient and safe, gene delivery vehicles called vectors have been created. The vectors being used are modified and attenuated viruses. The virus is modified in such a way that its disease causing component is removed and in its place gene are inserted. Synthetic vectors are also being used formed of complexes of DNA, Protein and Lipids.
The first human trials of Gene therapy began in 1990. Many types of diseases are currently being investigated as candidates for gene therapy including cardiovascular diseases, cholesterol lowering therapy, infectious diseases such as AIDS, and cancer.
Gene therapy can be used not only in treating genetic diseases but also to deliver specific proteins. By placing genes in laboratory-cultured organisms that produce the proteins coded by those genes. Examples of such manufactured proteins include insulin, growth hormone, and erythropoietin, all of which must be injected frequently into the patient.
In hemophilia treatments, a gene-carrying vector could be injected into a muscle, prompting the muscle cells to produce Factor IX and thus prevent bleeding. This method would end the need for injections of Factor IX — a derivative of pooled blood products and a potential source of HIV and hepatitis infection. In gene therapies such as these, the introduced gene is always “on” so the protein is always being produced, possibly even in instances when it isn’t needed.
|
First human chromosome mapped |
For the first time, scientists have mapped virtually an entire human chromosome, one of the chains of molecules that bear the genetic recipe for human life. The achievement was announced on Wednesday 1st Dec ’99. It was an important step for the $3 billion Human Genome Project, which is attempting to detail the tens of thousands of genes that carry instructions for everything in a human from brain function to hair color to foot size.
This is probably the most important scientific effort that mankind has ever mounted. That includes splitting the atom and going to the moon. In laying out the chemical instructions for life, scientists believe they are in the early stages of revolutionizing the study of human development and medicine. Already, researchers have begun testing several biological therapies that replace faulty genes or correct their misfirings to make cells work correctly. Such therapies, if they can be made reliable, would bring a more precise way to treat diseases without the sometimes debilitating side effects of conventional drugs.
The defects in the genes along the chromosome contribute to heart defects, immune system disorders, cancers, schizophrenia and mental retardation.
The human genetic pattern, or genome, is a biological map laying out the sequence of 3 billion pairs of chemicals that make up the DNA in each cell. All human DNA is contained within 23 pairs of chromosomes.
Genes are arrayed along chromosomes, the rod-shaped bodies inside the nucleus of a cell. Proteins and other compounds carry out the instructions of genes. Inside the chromosomes, genetic material is linked along tightly coiled strands of the master molecule DNA, which twists like a spiral ladder. Each rung is built with pairs of four chemical bases ordered in different numbers and combinations to form genes.
Mapping a gene is only an early step in understanding the gene’s function and how it might contribute to a particular disease.
Human Genome Genome Sequencing helps diagnosing rare disorder Genome Editing