Painful Sex |
| A large number of women are said to suffer from painful sex at some time or the other in their lives. In majority this remains unspoken and the women takes it that it may be a normal phenomenon or some think that they are alone with this problem. This condition is known as Dysparennia. Some amount of pain during sex is common and goes off after sometime.
Common causes of Pain during sex:
Vaginal Dryness – is one of the most common causes of pain during sex especially in young brides because of ignorance, insufficient arousal, inadequate foreplay, fear of pregnancy, stress or hormonal imbalance. Vaginismus – is a phenomenon in which the muscles at the vaginal opening constrict into tight spasm as soon as intercourse is attempted. This is a protective response against penetration and can happen specially with brides because of extreme fear, inhibition, improper sex education, childhood trauma, witnessing an unpleasant sexual activity. This results in a vicious circle of pain and fear. Vaginitis – is any type of vaginal infection or may be due to some allergic reaction or chemical irritation. The commonest is Thrush – a fungal infection resulting to foul smelling discharge. Lichen Sclerosis – is an auto immune condition in which immune cells attack the skin. It can affect any part of body, vulva is a common target. It usually develops after 40. Vulvadynia – In this condition there are nerve abnormalities around the vulva. It causes constant itching, burning pain around the vulva and vagina which worsens when touched even with water. Vestibulitis – In this condition too there is burning around vulva with redness and soreness. Tends to affect between 20s-30s. Cystitis – Most of the women experience this especially on the first initiation into sex. that is why it is also referred to honeymoon cystitis. It may also occur when sex is resumed after prolonged inactivity. It causes burning sensation while urination, frequent cloudy or bloody urine. Menopausal Thinning – This occurs with menopause when ovaries produce less estrogen resulting to vaginal lining thinning out and shrinking of the vagina. Endometriosis – In this condition the tissue that lines the uterus gets developed in other areas like fallopian tubes, ovaries abdominal wall or ligaments supporting the uterus. Women in 20s and 30s are most prone to this condition. It causes sharp pain deep in lower abdomen during intercourse. This condition may go after menopause or with hormonal therapy. Pelvic Inflammation Disease – It can cause following frequent chlamydia infection or infection following childbirth or due to IUD. Radiation scarring – due to radiation for cervical cancer or endometrial cancer can result in decrease in the length and circumference of the vagina because of adhesions and fibrosis. |
Category Archives: Diseases & Conditions
Chronic Granulomatous Disease
Chronic Granulomatous Disease |
| Chronic Granulomatous Disease is a rare disease. It is estimated to occur once in 250,000 individuals. Most often CGD is inherited as an X-linked recessive pattern, although in about 40 percent of patients the disease is inherited with an autosomal recessive pattern.
Patients with CGD characteristically have increased infection. When patients with CGD become infected, they often have extensive inflammatory reactions despite the administration of appropriate antibiotics. Aphthous ulcers and chronic inflammation of the nares are usually present. Granulomas are frequent and can obstruct the gastrointestinal or genitourinary tracts. |
| Blood in the placenta contains bone marrow stem cells. This fact was made use by the doctors to treat a rare disease known as Chronic Granulomatous Disease in a child. Dr. Andrew Cant, director of the children’s bone marrow transplant unit claim it is the first time the treatment has been used.July 04, 2002A 3-year-old north Wales boy, Tom Stretch with a life-threatening condition has been cured after a pioneering treatment involving his mother’s placenta. This child was suffering from CGD and needed a bone marrow transplant to combat a blood defect which had left him unable to fight off germs. The boy had a series of serious pneumonias and an inflamed bowel.
He needed bone marrow transplant and there was no immediately suitable bone marrow donor. After his mother Joanne gave birth to his sister Hannah at Ysbyty Glan Clwyd in north Wales in November last year doctors preserved the placenta. The blood was kept in a bank at Newcastle General Hospital’s specialist children’s bone marrow transplant unit. Doctors decided to try an infusion of the placenta blood containing the stem cells as an alternative to bone marrow transplant. The treatment to infuse the cord blood into the vein took place 16 weeks ago and experts claim that Tom’s condition has now been cured and he is free of infection and his bowel inflammation is settling rapidly. Its first time anywhere in the world that this technique has been used to treat CGD. |
Urticaria
| Urticaria | |
| Chronic Urticaria is common and extremely difficult condition.Chronic urticaria presents in a variety of presentation.About 5 % are shown to be Reactive to the food allergens.5% may have urticarial vasculitis.
Physical urticaria is seen in about 35%-40 %, aprox. 50 % have so called Idiopathic Urticaria. |
Epidemiological data available is scare. In UK about 1% of the population will suffer from urticaria during their lifetime. Out of this appox. 25 % of the patients would be of chronic urticaria.
|
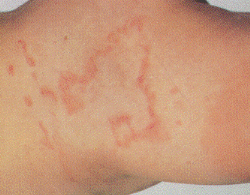
| Physical Urticaria: In this most striking is dermographism. A useful procedure in confirming the diagnosis of dermographism is challenge test with a calibrated dermographometer, which measures the pressure being applied to the skin.Other common physical urticarias are cold urticaria, cholinergic urticaria and solar urticaria. Cold urticaria can be tested by applying ice to the skin, cholinergic urticaria can be seen by exercising the patient or bathing in warm water and solar urticaria can be tested by solar simulator lamp. | 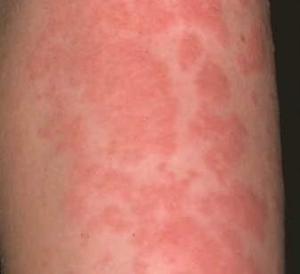 |
| Cold urticaria can be tested by applying ice to the skin | 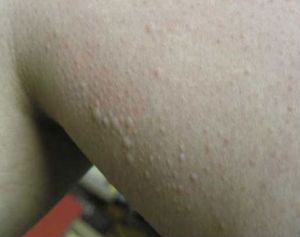 |
| Solar urticaria can be tested by solar simulator lamp.Patients with physical urticaria need no firther investigations. The patients shold be informed of the condition for which the average time course of 2-3 years, and during this time the main therapeutic approach is to cover the patient with H1 antihistamine. Very little is known about the pathogenesis of the physical urticaria. | 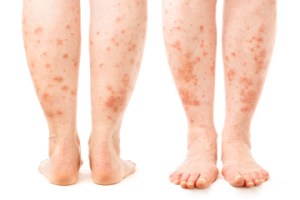 |
| Urticarial Vasculitis:In this the duration of the wheals is important. If the wheals last longer than the 24 hrs, the patient almost certainly has urticarial vasculitis. Staining of the the skin after fading of the wheals is another clue. Itching is not a major problem with this type of urticaria. The lesions are more likely to be tender and painful. The diagnosis of this type of urticaria is confirmed with skin biopsy. Another very important point to remember in this is that urticarial vasculitis may be a marker for serious systemic diseases involving kidneys, lung or cardiovascular system. It may be associated with hepatitis B or C. It may be first sign of autoimmune connective tissue diseases such as Sjogren’s syndrome, Systemic Lupus or Rheumatoid Arthritis. This condition is difficult to treat. Among the drugs useful are Dapsone, Colchicine, Indomethacin, Phentoxiphylline, Azathioprine, Corticosteroids.Food Allergens:A small proportion of the patients of chronic urticaria are allergic to food additives such as preservatives like Tartrazine and Sodium Benzoate, coloring agents and various antioxidants.
Parasitic infestations: May also produce urticaria especially in under developed countries. Chronic Idiopathic Urticaria: Autoimmune phenomenon appears to play part in in about 30-50% of the patients of Chronic idiopathic urticaria. Such patients have functional autoantibodies reacting with IgE receptor on the mast cells. |
|
|
Management Aggravating factors such as alcohol consumption, intercurrent infection, vigrous exercise and psychological stress should be kept in mind to understand why urticaria is at times worse. Antihistamine Treatment – Antihistamines such as Fexofenadine, Loratadine and Certizine. In patients uncontrolled with antihistamines, a short course oral steroids may have to be given. In some patients Cyclosporin for a period of 3 months may have to be given. |
|
| Skin Diseases | |
Hydrogen Cyanide
| Hydrogen Cyanide |
HYDROGEN CYANIDE, also called hydrocyanic acid and prussic acid, extremely poisonous, colorless liquid with a bitter-almond odor. The compound’s chemical formula is HCN. HCN melts at –14° C (6.8° F) and boils at 25.7° C (78.2° F).
It is reported that this substance was used by Iraq in the war against Iran and against the Kurds in the northern Iraq in the 1980s.A few milligrams of the substance and of related cyanides can be rapidly fatal to humans, acting by blocking the ability of cells to use oxygen. The compound mixes with water, alcohol, and ether in all proportions. When impurities are present, HCN molecules can combine to form a black solid; the reaction may be explosive unless inhibited. HCN is flammable and can form explosive mixtures with air. It was once produced from the pigment Prussian blue, hence its secondary name. Now it is prepared commercially by the reaction of methane with ammonia in the presence of a platinum catalyst. One major use of HCN is in the production of acrylonitrile, a starting compound for various products. HCN has many other industrial uses, including the making of plastics and several important cyanide compounds. The latter include sodium cyanide (NaCN) and potassium cyanide (KCN), both of them important in metallurgy. They are used in recovering gold and silver from ores, for example, and NaCN is used in the hardening of steel. Several cyanide compounds are employed in the electroplating of metals such as silver, gold, copper, and platinum. |
Cyanide Poisoning Chemical Weapons
Hepatitis
Hepatitis |
| Hepatitis is a type of Liver disease. Most commonly caused by viral infections which are of different types – Hepatitis A virus, B virus, Delta virus, C virus, Non-A, Non –B virus, Cytomegalovirus, Epstein-Bar virus, Herpes simplex virus, Yellow fever virus.
Hepatitis A virus Is highly infectious. Spreads by faeco oral route. Poor sanitation aids in its spread. In occasional out breaks water, milk, and shellfish has been the source of spread. In this form a carrier state does not exist. The disease is usually mild as compared to Hepatitis B infection. Hepatitis B virus In this type of hepatitis the main source of infection is blood, and the spread my follow transfusion of infected blood or blood products or infection with contaminated needles. Tattooing and acupuncture can also spread this disease. Close personal contacts such as sexual intercourse and especially in the homosexuals is also an important cause of infection. It can be also spread to child from mother at or soon after birth. Hepatitis B vaccines are available to protect against this infection. This vaccine is ineffective in those already infected with this disease. Vaccination against Hepatitis B forms part of compulsory vaccination of infants in the first year of life. Three doses are needed at 0, 1 and 6 months interval. Hepatitis B infected individuals carry this infection throughout life. Some are just carriers without having any symptoms of any illness. Some may have acute illness and some develop chronic liver diseases. These persons are at a much high risk of developing Liver cancer in later life. Delta virus The delta virus is an RNA containing partial virus which has no independent existence. It requires the hepatitis B virus for replication and has the same source and mode of spread. It causes progressive chronic hepatitis and eventually cirrhosis. Non-A, Non-B, C and E viruses Non-A, Non-B and C hepatitis is caused by several viruses. The mode of transmission in humans is similar to those of hepatitis B virus. In developed countries Non-A and Non-B & C hepatitis is now cause of 90 % of the post transfusion hepatitis. It can also be spread by other blood products. Hepatitis E virus is an entericlly transmitted virus that occurs primarily in India, Asia, Africa, and Central America. This agent has epidemiologic features resembling those of hepatitis A. The virus has been detected in stool, bile, and liver from infected patients as well as from experimentally infected nonhuman primates. Studies in humans and experimental animals have shown that HEV is excreted in the stool during the late incubation period. The commonly recognized cases occur after contamination of water supplies such as after monsoon flooding. An epidemiologic feature that distinguishes HEV from other enteric agents is the rarity of secondary person-to-person spread from infected persons to their close contacts. In outbreaks of waterborne hepatitis E in India and Asia, the case-fatality rate is 1 to 2 percent and up to 10 to 20 percent in pregnant women. The most feared complication of viral hepatitis is fulminant hepatitis (massive hepatic necrosis). |
|
Hepatitis B Vaccination |
| Until 1982, prevention of viral hepatitis-B was based on passive immunoprophylaxis, either with standard IgG containing modest levels of anti-HBs or hepatitis B immune globulin (HBIG) containing high titre of anti-HBs.
Initially the vaccine for active immunisation was prepared from the plasma of healthy HBsAg carriers. The vaccine was subjected to 3 different chemical inactivation steps which cumulatively destroy the infectivity of every known virus without harming the host. The plasma derived vaccine in 1987 was substituted by the genetically engineered vaccine derived from recombinant yeast. This genetically engineered vaccine (Engerix B and Recombivax – HB) consists of HBsAg particles that are non- glycosylated but is otherwise indistinguishable from natural HBsAg. It is equally immunogenic, protective and safe as the first generation plasma-derived vaccine. Indications for hepatitis B vaccination include pre-exposure and post-exposure cases. Pre-exposure prophylaxis is advised in the following cases:
Pregnancy is not a contraindication for hepatitis B vaccination. Site of administration: The vaccination is indicated at 0, 1 and 6 months in the deltoid region or the anterolateral aspect of the thigh and not in the glutial region as it may reduce the efficacy of the vaccine. Dosage: 1 . Engerix B. (i) 10 micog in children below 10 years; (ii) 20 micog for immunoincompetent children below 10 years; and Adults. (iii) 40 micog for patients on dialysis and other immuno- compromised persons. 2. Recombivax-HB. (i) 2.5 micog for children below 11 years of HBsAg-negative mothers; (ii) 5 micog for infants of HBsAg-positive mothers and children and-adolescents between 11 and 19-yrs; (iii) 10 micg for immunoincompetent adults; and 40 micog for patients on dialysis and other immunocompromised persons. 3. Heppacine-B (plasma derived): 1 ml IM at 0, 1 and 6 months. For unvaccinated persons sustaining exposure to HBV, treatment comprises: 1. HBIG for immediate action. 2. Hepatitis B vaccination for prolonged action. Special precautions: One should be careful during febrile illness infections and in patients on immunosuppressive therapy. Adverse side effects may include: tenderness and indurations at the site of the injection, fatigue, fever, headache, dizziness and arthralgia.
|