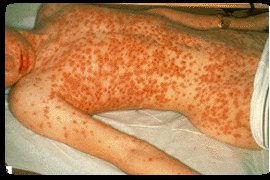
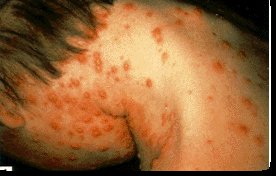
Eczema |
There are two types of Eczema:
Exogenous or Contact Eczema
Endogenous or Constitutional Eczema
|
CONTACT ECZEMA |
IRRITANT CONTACT ECZEMA
Detrgents, alkalis, acids, solvents and abrasive dusts are common causes of irritant contact eczema. Majority of industrial irritants causing contact dermatitis come under this category. Those with fair dry skin and with a family history of allergic diseases such as asthma, hay fever or eczema are more vulnerable to irritant contact dermatitis. Napkin eczema in babies comes under this type of eczema.
ALLERGIC CONTACT ECZEM
It is due to delayed hypersensitivity reaction to a contact with an antigen. Previous exposure to antigen is required for sensitization to occur and the reaction is specific to the antigen or closely related chemical.
COMMON ALLERGENS :
Nickel: Jewellery, jeans studs, bra clips.
Dicromate: Cement, leather, matches.
Rubber: Clothing, tyres, shoes.
Colophony: Sticking Plaster.
Paraphenylenediamine: Hair dye, Clothing.
Balsum of Peru: Perfumes, Citrus fruits.
Parabens: Preservatives in cosmetics and creams.
Wool Alcohols: Lanolin, Cosmetics, Creams.
Epoxy Resins: Resin Adhesives.
Topical Applications: Neomycin, Benzocain
|
|
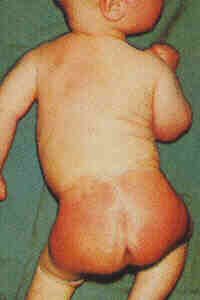
Diaper Dermititis
Moist, bright red lesoins over the diaper area sparing the inguinal flexures. Setellite lesions may be seen. Treatment : Area to be kept dry. Topical antifungal – steroids creams or lotions. |
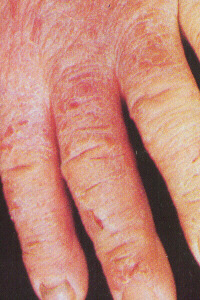 |
Hand Eczema
Excessive exposure of hands to soaps, chemicals etc. causing redness, scaling and fissuring. Treatment : Avoidance of causative factors, Topical steroids-antibiotic preparations. |
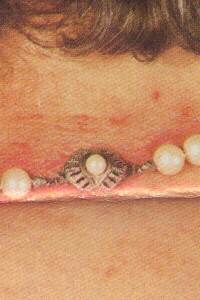 |
Contact Dermatits
Erythematous, oozing, crusted lesions occurring at the site of contact with metals (earrings, wrist watches, necklaces etc.) Treatment : Avoid contact with the allergens. Topical steroids creams or lotions. |
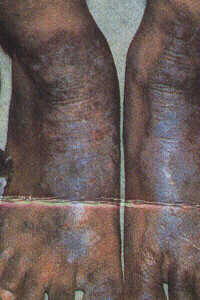 |
Foot Wear Dermatitis
Erythema and oozing, or lichenification seen on the dorsal aspects of feet. Depigmentation may also occur. Treatment : Topical steroids, change of footwear. |
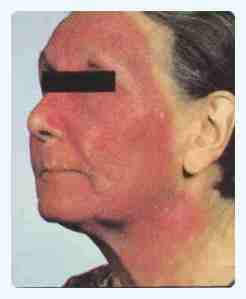 |
PhotoContact Dermatitis
Itchy, erythematous, scaly and or fluid filled lesions seen on the exposed areas of the face, neck, back of the hands etc. Treatment : Avoid photosensitizing agents, Use steroid topically and sun screening agents. |
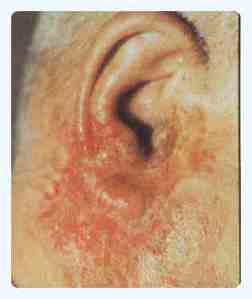 |
Microbic Eczema
Sensitizaton to causative organism leads to oozing, crusted eczematous lesions around the primary lesion. Treatment : Local cool compress, topical steroid-antibiotic cream,systemic antibiotic. |
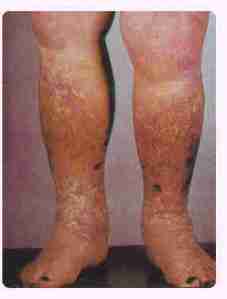 |
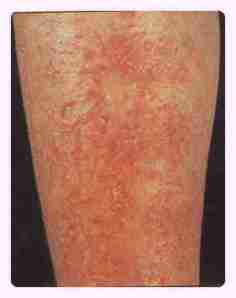
Stasis Eczema
Pruritic, weeping and eroded lesions seen on the lower leg. Varicose veins usually present. Treatment : Leg elevation , wet compresses, systemic antibiotics and topical steroids. |
 |
Xerotic Eczema (Dry Skin)
Skin is dry and flaky especially over the arms and legs with generalised pruritus. Treatment : Infrequent bathing; avoid soaps; Urea cream, vaseline or cold cream. |

 and in rainwater that collects in various containers (e.g. tyres, bottles, tanks, shallow wells, plastic bottles.)
and in rainwater that collects in various containers (e.g. tyres, bottles, tanks, shallow wells, plastic bottles.)
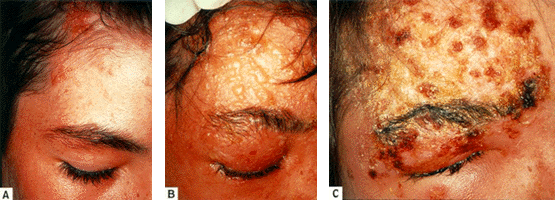




 febrile throughout the evolution of the rash and experiences considerable pain as the pustules grow and expand. Gradually, scabs form, which eventually separate, leaving pitted scars. In severe cases death usually occurs during the second week.
febrile throughout the evolution of the rash and experiences considerable pain as the pustules grow and expand. Gradually, scabs form, which eventually separate, leaving pitted scars. In severe cases death usually occurs during the second week.