| Molluscum Contagiosum | |
| Molluscum contagiosum is a skin disease. It is generally a benign disease characterized by pearly, flesh-colored, umbilicated skin lesions 2 to 5 mm in diameter. It is caused by a Poxvirus. The infection can be transmitted by close contact, including sexual intercourse. Lesions typically occur in the genital region but can be found anywhere on the body except the palms and the soles. In most cases the disease is self-limited and has no systemic complications. |
 |
| Mulluscum contagiosum develops often in cases with the advanced stages of HIV infection. 5 to 18 percent of HIV-infected patients develop this complication. The disease is more generalized and severe in AIDS patients with frequently involving the face and upper body. | 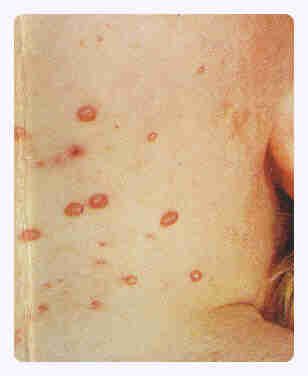 |
| There is no specific systemic treatment for molluscum contagiosum, but a variety of techniques for physical ablation have been used such as Electocautry, chemical cautry, Trichloroacetic acid applications or Liquid nitrogen applications or Light electrosurgery. | 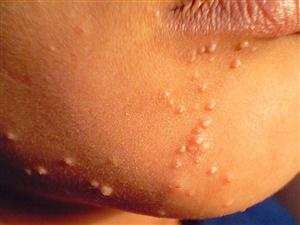 |
| Skin Diseases | |
Author Archives: Manbir & Gurpreet
Menorrhagia
| Menorrhagia ~ Excessive Menstrual Bleeding |
| It is one of the most common menstrual disorders and is called Menorrhagia. It affects about a third of the women. A woman who bleeds for more than 10 days or women who uses more than 10 pads a day may be labelled as suffering from Menorrhagia.
Causes:
Women due to excessive bleeding develop anaemia. It leads to deterioration of general health which lead affects family and social life. Dysfunctional Uterine bleeding is abnormal uterine bleeding caused by interruption of normal ovarian functions that produces eggs called ovulation. Tests are performed to evaluate the status and cause of the bleeding. These include blood tests, ultrasound examination, Pap smear, D&C, and Hysteroscopy. Women who experience single episode of heavy bleeding may not need much treatment but those who get heavy bleeding for more than 24 hrs need to seek medical advice. Relief from menorrhagis is achieved by treating under lying causes. Often it is managed with progesterone or a combination of progesterone and oestrogen as in the form of oral contraceptive. |
Benefits of Sex
Quote
|
Benefits of Sex |
|
| In a study done to find out the relation between Sex and Cardiovascular benefit it was found that those who have regular sex do get some cardiovascular protection. This benefit was seen in a group who had sex in a married relationship and not among those having casual sex outside marriage. |
Hormone Replacement Therapy (HRT) ~ Risks
| Risks of Hormone Replacement Therapy (HRT) |
| Two major studies created lot of the furrow and confusion among a large population of women and medical professionals. The first, Women’s Health Initiative (WHI), was called off after Prempro, a popular estrogen and progesterone combination therapy, was shown to increase risk of stroke, heart disease and breast cancer in post-menopausal women.The second, being conducted by the National Cancer Institute (NCI), showed that post-menopausal women who took estrogen had a 60 percent greater chance of contracting ovarian cancer than did women who took no hormones.
Estrogen products have been used for decades and have helped millions of women handle symptoms of menopause, including hot flashes, night sweats, sexual discomfort and the increased risk of bone fractures. For years, studies on heart disease, Alzheimer’s, colon cancer and bone fractures also showed potential benefits to women taking hormone replacement long-term, and these findings were widely accepted by doctors and advertised by the drug makers. The findings regarding the benefits of estrogen on heart disease were considered strong enough by the American Heart Association to be included in its literature for women as recently as 1997. But all this has changed over night with the findings of WHI. Researchers running the federally funded Women’s Health Initiative announced that the largest U.S. trial of combination hormone therapy in healthy postmenopausal women had been stopped three years early because of an increase in breast cancer cases among hormone users. Increases in heart attacks, strokes and blood clots also led the oversight committee to halt the study. Overall, the researchers concluded that the treatment was hurting the test subjects more than it was helping them. That assessment applied to women taking estrogen and progestin, but not to women in a separate study evaluating the use of estrogen alone. Researchers said that they had not detected any significant increase in breast cancer among women taking estrogen only and that the study would continue. Experts say, women who are taking the hormones should not panic, but should consult with their doctors about whether to continue. It is advised that women who take the two hormones to relieve hot flashes and other symptoms of menopause should use the treatment as briefly as possible, and those wishing to prevent osteoporosis should probably choose alternatives to hormones. Also, the result of this study on the use of contraceptive is unclear for the present. The observations of this study has no bearing on the use of contraceptive pills by women of pre menopausal age. This study was conducted with Prempro. Prempro is taken all month, while oral contraceptives are prescribed to be taken for three weeks, then stopped for one week — to mimic the body’s natural hormonal cycle. Some think this cycling may be protective. |
| Findings of WHI in relation to HRT |
Following are the observations out of the Women’s Health Initiative study:Before stopping its eight-year study at the five-year mark, the WHI came to the following conclusions:
There was no difference in death rates between the two groups. However, women on the hormone treatment had a
In contrast, the hormone-treated women
The study found that the frequency of these effects in hormone users did not differ by age, ethnic group or prior health status. |
Menopause
|
Menopause |
| The menopause is defined as the final episode of menstrual bleeding in women. The term is used commonly to refer to the transitional period up to and after the last episode of menstrual bleeding. During this period, there is a progressive loss of ovarian function and a variety of changes due to hormonal upset.The median age of women at the time of cessation of menstrual bleeding is 50 to 51 years. In the 5 years before menopause there is gradual increase in the number of anovulatory cycles – i.e. cycles without ovulation. During this period the estrogen secretion falls and there is increased pituitary secretion of LH and FSH hormones. The age of menopause varies widely. Before the menopause the interval between the menses is variable and it becomes longer and longer.The menopause is the consequence of the exhaustion of folicles in the ovaries of a female. The decrease in the number of ova begins in the womb itself. By the time of the menopause, few ova remain, and these appear to be non-functional. Only a small number of ova are lost as the result of ovulation during reproductive life. The stopping of follicular development results in decreased production of estradiol and other hormones.Estrogen and androgen levels in plasma are reduced but not absent. |
|
Many factors affect the development of osteoporosis, including diet, activity, smoking, and general health, and estrogen deprivation is of particular importance. White postmenopausal women are more predisposed to osteoporosis and its consequences. It is known that fall in the secretion of estrogen is associated with initial rapid loss of bone mass. Vertebral compression fracture, fracture neck femur and radius is seen more in females in comparison to males. Those women who smoke are at a greater risk. Excessive alcohol and lack of exercise add to this risk. Earlier the menopause greater is the problem. Oestrogen started at the time of menopause is shown to prevent the bone loss. Many factors affect the development of osteoporosis, including diet, activity, smoking, and general health, and estrogen deprivation is of particular importance. White postmenopausal women are more predisposed to osteoporosis and its consequences. It is known that fall in the secretion of estrogen is associated with initial rapid loss of bone mass.
|
|
Management
Oral Oestrogen – cyclical Ethinyl oestrogen 0.01-0.02 mg / day for 21 days with Medroxyprogesterone acetate 5 mg daily for the last 10 days. Percutaneous Patches with reservoir of oestradiol 25-50 µg / day. Change every 3-4 days. Add oral Progestogen for 10 days per month. Topical oestradiol – for Atrophic Vaginitis 0.01 % Dienoestrol cream.
|